About this Page
|
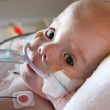
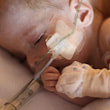
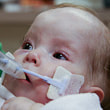
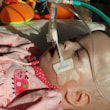
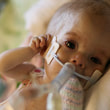
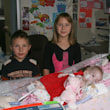
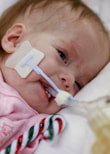
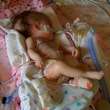
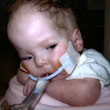
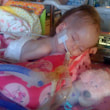
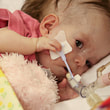
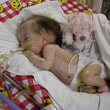
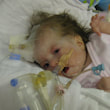
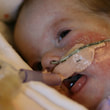
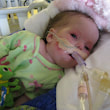
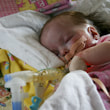
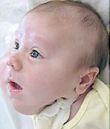
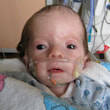
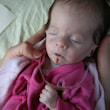
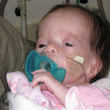
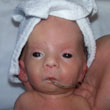
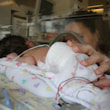
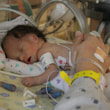
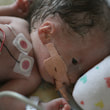
This is a "blog" about Hailey's story. It was originally intended to keep our family and friends updated on her progress and diagnoses. Now it's a tribute to her… her story, her fight and her life.
In the beginning, we planned to update it frequently, then taper off to major milestones. You won’t hear about every pee or poop – although some may have been considered major milestones. This page is written with the latest stuff is at the top and earlier stuff at the bottom. So if this is your first time reading it, start at the bottom and work your way up. |
March 29, 2010
|
This morning was the celebration of Hailey’s life. She was laid to rest in the Garden of Angels at Glen Eden Memorial Gardens.
We would like to thank all of our family, friends and colleagues for all of your love, support and encouragement, not just over the past week, but over the past 10-1/2 months. Your cards, email messages and voicemail messages have made us cry, laugh and everything in between. You have made us realize how much Hailey is loved and how much everyone was “cheering” for the three of us from the “sidelines”. Thank you!! Hailey’s eulogies are below (click on each one to view them):
|
March 27, 2010
March 24, 2010
March 23, 2010
|
This morning, with our hearts in our throats, we said good-bye to Hailey. She passed away peacefully in our arms and surrounded by our love. God bless you our sweet little angel. We love you to the moon and back, forever and ever and always. You will always be in hearts, our thoughts and our prayers.
|
March 15 - 22, 2010
|
Through the months, Hailey has fought many, many, many battles, and has never fully recovered from any of them. Over the past couple of weeks Hailey’s health quickly deteriorated and she required more and more and more support. On Sunday, after counseling with Hailey’s nurse and the NICU Attending, we decided that it was no longer fair to ask Hailey to keep fighting. It’s the right time to say good-bye and free her of all tubes, wires, and “beeps and boops” that have been her life.
|
March 8 - 14, 2010
|
We weren’t sure what to expect on Monday – Hailey had such a good evening on Sunday. We just hoped that it continued through the night and into the morning. It did!! …until about lunch time. To quote Janet, “The afternoon went to H, E, double hockey sticks in a hand basket!!” Hailey started to wake up shortly after noon, but unlike Sunday evening, she didn’t wake up so cheerfully. They thought that she was fighting the Jet and that it might be time to try her back on the conventional ventilator. She fought it tooth and nail for some time, but finally after many tweaks to her vent settings… and some “happy” drugs, she finally settled down. During the evening, she had some nice awake periods with us – especially since she no longer needs to be paralyzed. She even gave us a few smiles!!! (this caused her mom and dad’s eyes to leak)
|
|
March 1 - 7, 2010
|
This was a week from H, E, double hockey sticks!!!
Monday was more of the same (as last Sunday)… increased heart rate, high temperature, restless – but she did have periods where she smiled and looked really good. We also received preliminary results that Hailey had a septic blood infection (not good). On Tuesday, her nurse collected and sent off more blood to be tested – this time, one sample from each of her central lines. Tuesday during the day was pretty much the same as Monday. However, by later afternoon, things rapidly changed. Hailey’s oxygen requirements started to get really high and she was working harder and harder to breathe. Since Monday afternoon, she also started to look puffier in the eyes (edematous). We discussed giving her more Lasix, but the Fellow wanted to do a blood gas test and a chest X-Ray. The X-Ray looked fine, but the blood gas showed that Hailey’s CO2 in her blood was really, really high (nearly 100 mmHg). They tried hand ventilating her for a while – hand ventilating is more efficient at “blowing off” the CO2 than the ventilator – but it didn’t help. Also, Hailey’s FiO2 was super high – at 100%. A short while later, after another bad blood gas, they decided that it was time to change her to a High Frequency Jet Ventilator (a.k.a. “the Jet”). The Jet breathes little puffs at a very high rate (360 times per minute – or 6 times per second!!). The Jet is more effective at “blowing off” CO2 – as one of Hailey’s nurses put it, “the Jet could get CO2 out of a stone”. As predicted, Hailey responded very well to the Jet but she was still having issues with her oxygen requirements. Because of Hailey’s rapid deterioration and slowness to recover, there was also a concern that this also could have been a pulmonary hypertensive crisis (like she had in August) – so just in case, they re-started her on iNO (inhaled nitric oxide). The Respiratory Therapists (RT’s) and Physicians spent quite some time tweaking the Jet. They can’t “blow off” too much CO2 or else it changes her blood chemistry too much. One of largest downsides of the Jet (as parents) – besides Hailey being so sick that she needs the Jet – is that Hailey needs to be completely paralyzed and sedated while she’s on it – or else she would be fighting it and would be too uncomfortable. By 2:00 a.m., Hailey was stable enough that we felt somewhat comfortable to go home for a few hours. Wednesday morning they started to rule a few things out. They did a cardiac echo to confirm her cardiac status – there was no PPHN (so her iNO was turned off). Also with the echo, they were able to rule out a pulmonary embolism. And, they also ruled out “septic shock”. Later in the day, they started to refer to Hailey’s condition as “Acute Respiratory Distress Syndrome” – basically a condition where, because of her septic blood infection, her respiratory system just “shut down”. Through the day, Hailey also had bouts of really low blood oxygen saturation levels – mostly associated with moving her or suctioning secretions out of her lungs. These bouts were concerning because her blood oxygen saturation level dropped so low and she took such a long time to recover. To help with this, they decided to put her back on iNO – this time not because of PPHN (pulmonary hypertension), but because iNO is a good vasodilator and helps oxygenate the blood. Wednesday was Colin’s birthday. In the evening the nurses surprised him with a card and a cake… he turned 25 this year!! 😃 The rest of the week was spent tip-toeing around Hailey – trying not to upset her too much, but still trying to tweak her ventilator settings. They also wanted rule out a few more things – like if she was having seizures – so they did an ultrasound of her head and a lengthy EEG study. Both came back negative. We’re in it for a long haul – it will likely take us several weeks to get back to where we were last week…(sigh) But as each day passes, we can see improvements; each day Hailey can tolerate more and more – more suctioning, more movements. Also each day, the nurses try to stretch out the time between when they give Hailey her paralysis drug because it causes a buildup fluids in her tissues (edema). On Sunday night, Hailey treated us to a very long period of being awake (by this week’s standards at least). After turning her and suctioning her, Hailey was awake and alert for almost 2 hours. Baby steps… |
February 23 - 28, 2010 (Back in Winnipeg)
|
The rest of the week was spent getting Hailey “dialed” in.
To suit some of the changes that were made with Hailey’s ventilator settings in Edmonton, and because the ventilator that was used in PICU in Edmonton is different than the ventilator used in NICU in Winnipeg, they had to “tweak” her ventilator settings over several days until Hailey was “reacquainted” with her old ventilator. As part of the changes that were made in Edmonton, we increased her Total Fluid Intake (TFI) in an attempt to increase her caloric intake and get her back on track to gaining some weight. As we began to learn in November and December, Hailey is very sensitive with her fluid balance – too much or too little, and she gets into trouble. Luckily, starting after Christmas and until we left for Edmonton, Hailey was pretty stable with respect to her fluid balance. Due to them increasing her TFI, they had to supplement Hailey’s regular diuretic, Aldactazide, with once a day Lasix (another diuretic). Also in an attempt to further increase Hailey’s caloric intake and to keep her tummy empty to help heal her GT site (stoma), we stopped feeding her through her new NJ tube. Hailey would get all of her nutrition through her, also new, PICC line. On Sunday, Hailey started to “spike” a temperature. She also had a higher heart rate and was quite a bit more fidgety. Is this another fever coming her way?? They drew some blood samples, urine samples, etc., etc. and started her on antibiotics. |
|
February 15 - 22, 2010 (Edmonton)
|
February 15, 2010 (Monday)
We were told last week that PICU (Pediatric Intensive Care Unit) in Edmonton would likely not have a bed for Hailey on Monday (as originally scheduled). Through the weekend, although Edmonton wouldn’t commit, it looked a little more promising that they might have a bed, but said that they would call NICU (Winnipeg) Monday morning. So…Monday morning, after a late night packing and getting everything else ready, we received a call from “Auntie” Catherine (Hailey’s daytime “Auntie” and nurse) – it was a “no go” for at least Monday and we would try again Tuesday. February 16, 2010 (Tuesday) Tuesday…same drill…but this time we were somewhat surprised when Catherine told us that we were going. Hailey was scheduled to leave between 1:30 and 2:00 in the afternoon…but this got pushed back to 3:00. With much fanfare, and under the watchful eyes of her gallery of well-wishers, Hailey and her entourage of 5 (“Auntie” Catherine, Dr. Caces, Jeremy the RT…and 2 Paramedics to transport them) left for the airport. We had originally planned on going to see them off, but we had our own plane to catch...and by this time we were running late – we still had to go home to pickup our luggage and meet Janet’s dad who was going to give us a lift to the airport. By this time, Sedona (the cat) was already at Colin’s parents and Higgins (the dog) was at Colin’s sister’s - each for their own vacation. Hailey’s flight was direct (with no security checks, no waiting for luggage, etc., etc.)…and landed at Edmonton’s City Centre Airport (10 minutes from the hospital)…whereas our flight had a 45 minute layover in Calgary and landed at Edmonton’s International Airport, some 30 km away from the hospital. Needless to say, Hailey was well settled and tucked into bed before we even made it to Edmonton. Thankfully she had an uneventful flight and woke up just briefly to say “hi” and take in the sights and sounds of her first plane ride. Our flight landed shortly after 9:00 p.m., and after making our way to the hotel, we walked over to the hospital. Since we arrived “after hours”, it was a tad challenging trying to find our way to PICU…but we did. We arrived to find Hailey bright eyed, sitting up in her bed and looking around at her new surroundings. Shortly after, Hailey started to fall asleep, so we made our way back to the hotel to scrounge for a late supper, get settled into our hotel room, and go to bed. February 17, 2010 (Wednesday) After a scant 5 hours of sleep, we were awakened by a telephone call from the hospital. They needed our consent to take Hailey for a chest and head CT scan. By 11:00, Hailey had her CT scan and was back in PICU. But we soon learned that this was just the beginning of a flurry of activity today. Besides numerous doctors and specialists coming to poke and prod her and ask us about her history, Hailey also had a cardiac echo, Doppler ultrasounds of her neck and groin (to check for access for her second heart catheterization) and an EKG. Also in preparation for her heart cath, they wanted to wean Hailey off of the iNO – from 20ppm to nothing by 8:00 the next morning – really, really quick by what we’re used to. Considering all of the activity and changes with her surroundings and the people around her, Hailey’s been handling these days like a real champ. Although only sharing sparse smiles, she’s in good spirits, and awake and alert most of the time. Just like at home, she’s winning everybody over with her big, beautiful, expressive eyes. By early evening, we were all exhausted. So after kissing her goodnight, we made our way back to the hotel for an early evening. February 18, 2010 (Thursday) This was Hailey’s big day…the day of her heart catheterization. Hailey was scheduled to be the third of the day – meaning that it would likely be sometime between noon and 2:00pm. Our champ is doing great!! We normally cringe at change. Hailey usually has her own plans when we go through too many changes too quickly. But the last few days, she’s been rolling with them…so far? Wednesday afternoon, they commenced rapidly weaning Hailey off the iNO. By midnight, she was down to 1ppm (a minimal setting) and she stayed at 1ppm for the remainder of the night. At 8:00am, the iNO was turned off, and she didn’t miss a beat. At 10:00, they did another cardiac echo to confirm that nothing has changed since her iNO was turned off – it hadn’t. Late in the morning, PICU had to be closed to ALL visitors – including parents!! - meaning we had to leave. They did a major procedure on another patient right in the unit, and everybody had to leave until it was finished. So we went to do some grocery shopping and have lunch. By the time we got back, the unit was re-opened and it was almost time for Hailey to leave for her heart cath. We had a short bedside talk with the anesthesiologist then she was off…and we waited and waited and waited… in all it took 3-1/2 hours. Dr. Adatia, Hailey’s Pediatric Cardiologist in Edmonton and the reason why we came, sat down with us for a lengthy, very friendly discussion on how the heart cath went and what he saw. In short, it went very well and he was impressed by what he saw. The pressures in Hailey’s heart were great – going as far as calling them “normal” – meaning that the drugs that Hailey’s currently on are working. He doesn’t see a need to continue with the iNO, but would like to continue with the Epoprostenol and Sildenafil at least until she is extubated. Before the heart cath, they inserted a “peripherally inserted central catheter line” (PICC line) into her left arm. This gave them more dependable IV access during the procedure and will stay in for as long as we need. In the short term, it’s good – since we lost her GT (we’ll update that story soon), Hailey’s been getting her nutrition (called TPN and Lipids) by IV. But because she’s only had a peripheral IV (a standard IV) for everything but her Epoprostenol, her TPN has been a lower concentration than what she really needs to gain any kind of weight – a higher concentration can’t be used in a peripheral IV. So until we get the GT thing sorted out, we can use the PICC line to give her a higher concentration of TPN. For some time, Hailey’s had quit a leak around her ETT. So also during the heart cath, they changed her ETT to one that has a small balloon-like cuff near the bottom end of it. The cuff on the new ETT can be inflated to control the leak. Hailey was pretty sedated for the heart cath, so she was still pretty dopey during the evening. She opened her eyes long enough to say “hello”. February 19, 2010 (Friday) WE’RE COMING HOME!!! …soon (likely Sunday) Relatively speaking, today was quiet. Upon discussions with Dr. Adatia and other “intensivists”, we decided not to do a bronchoscopy. We will wait until Hailey is a little closer to being extubated. They only did 2 small procedures today. The first one, Hailey slept through – it was, we think, called a metabolic test. All she had to do was breath…and sleep. It measures how much oxygen she was breathing in and how much carbon-dioxide she was breathing out. It gives an indication of how many calories she needs. That will help tailor her feeding requirements. The other procedure involved another road trip - this time down to the diagnostic imaging unit to insert a nasal jejunum tube (NJ tube) under fluoroscopy. This will be how Hailey will be fed until we figure out what to do with her GT. The jejunum is the middle section of the small intestine – after the stomach is a short section of small intestine called the duodenum followed by the jejunum. And fluoroscopy is real-time moving x-ray images, and was used to help them guide the tube into the jejunum. We joked that the next time Hailey left PICU, we were going to West Edmonton Mall. Once the NJ was in and we were back in PICU, they started feeding her again – the first time in almost 2 weeks. They will start with a very small amount, then ramp it up over the next day or so. We also decided to try a new formula called Neocate. Late in the afternoon, Dr. Aditia spoke with Dr. Seshia in Winnipeg. We all decided that Sunday would be a good day for Hailey to come home – as long as Winnipeg can make the arrangements, has staff for the flight and an aircraft is available. February 20, 2010 (Saturday) Hailey had a pretty calm day. No tests. No procedures. The only down side is that she was pretty unsettled for much of the day. February 21, 2010 (Sunday) CHANGE OF PLANS…We’re not coming home today. We were abruptly awakened shortly after 6:00am with a call from PICU. As Hailey was being repositioned for an x-ray, her heart rate and blood oxygen saturation dropped – to the point that she needed chest compressions and hand ventilating (bagging) for a short period (approximately 45 seconds). This was very similar to the 4 or 5 episodes that she had between the middle of November and the beginning of December. When the Attending Intensivist arrived, we discussed our options – to transport Hailey home today, or to watch her for the day and reassess Monday morning. Based on what happened and how quickly Hailey recovered, the Attending was pretty confident that this was “simply” a vagal nerve response – meaning that likely her ETT pressed against her vagus nerve at the back of her throat as she was being repositioned. This caused her heart rate to drop. Most people would be able to recover quickly, but because Hailey’s “reserves” are low she doesn’t have that luxury. Upon discussions between the Attending, Dr. Adatia and us, we all decided that it would be best to stay put for the day. We also decided that it wouldn’t hurt to do another cardiac echo to confirm that Hailey’s cardiac status hadn’t changed. It hadn’t. They also checked the gases in her blood – they did a blood test immediately following the episode and another about 30 minutes after. They showed that Hailey recovered pretty quickly. For the remainder of the day Hailey was pretty restful. She spent most of it sleeping and watching cartoons. It took that long for our hearts to get out of our throats. (sigh)…The roller coaster ride continues… February 22, 2010 (Monday) The waiting game begins… After packing our stuff at the hotel room, we made our way to the hospital. It was confirmed…Hailey was cleared to go. She remained stable for the remainder of Sunday night. In the morning the intensivists decided that there was no reason to keep her in Edmonton any longer. The NICU (Winnipeg) transport team would be leaving from Winnipeg at 1:00 p.m. …although we weren’t sure if that meant leaving HSC at 1:00 or taking off at 1:00…or if it was 1:00 Winnipeg time or 1:00 Edmonton time… Our flight was scheduled to take off at 6:30 p.m. – that meant that we needed to leave for the airport by 4:30. By 3:00 we’re nervously watching the clock and the door. Shortly before 4:00, we finally got word that the transport team was at the airport – but at the WRONG airport. Due to the weather, they had to land at the International Airport (45 minute drive), instead of the City Centre Airport (10 minute drive). We didn’t want to leave for the airport without knowing that Hailey was safely on her way too… but had to – we were running out of time. Reluctantly, we returned to the hotel to collect our bags and leave for the airport. Once we got to the airport, we called back to the hospital to confirm that Hailey was on her way… she wasn’t!!!! Just as the transport team was getting into PICU, Hailey had another vagal nerve response. They had to do chest compressions and had to hand ventilate her…again. Hailey’s beside nurse told us that they were doing some blood tests and a chest x-ray to help them make a decision whether it was safe for her to travel or not. She told that she would call us back in 10 minutes. After 35 minutes, by this time we were “crawling up the walls”, she called to let us know that Hailey was on her way. The blood test and x-ray showed that everything was normal and that she was cleared to travel. That helped our nerves very little!! A short time later, we got a call from Susan, the Winnipeg transport nurse with Hailey) to let us know that Hailey was stable and that they were in the ambulance and on their way to the airport. It was a very, very long trip home… Needless to say, we went straight from the airport to the hospital. We were pleasantly surprised to find Hailey back in her old spot – Bed No. 11 in Module C. She made it safe and sound. A day with yet another bump on the roller coaster... |
January 4 - February 14, 2010
|
Oops!! We’re a tad behind with our updates! Stay tuned…we’ll update these weeks shortly.
Not much happened, except that we (us and the docs in NICU) decided that it would be beneficial for us to go to Edmonton – specifically to the Stollery Children’s Hospital at the University of Alberta – for some tests and a second opinion…or better yet…a “fresh set of eyes”. |
December 28, 2009 – January 3, 2010
|
Yikes!! 2010 already!! Who woulda’ thunk that we’d still be in NICU.
Hailey continued to improve throughout the week. While sleeping her FiO2 was often 27-29% and while awake, 32-35%. She was almost back to her old-self – sharing smiles – although more for the Nurses than for her parents! On Tuesday, she popped out another tooth - her second on the top and her fourth overall. She’s showing more signs of teething (fever, increased heart rate, drooling, etc.) so we expect that more are on the way shortly. Thursday night, after dinner with some family and friends, we “rang in” the New Year with Hailey and our NICU family. Although Hailey continued to party through the night, which lead to an unsettled Friday. We hoped it’s just because Hailey was over tired and that it’s not leading something else. As it turned out, it was nothing. The rest of the week, Hailey did even better. Her FiO2 was really good – to levels that we haven’t seen since July!! (23-25% while asleep and 28-25% while awake) We hate to be pessimistic, but when things are this good, we keep expecting “the other shoe to drop”. We can only hope that these days are a trend and not just a “blip”. Either way, we have to enjoy theses good days as we get them. |
December 21 - 27, 2009
|
Monday was a bad day - Tuesday was even worse. Without sugar coating it, we weren’t sure if Hailey would be around to meet Santa Claus. At times, she was breathing pure oxygen – and it still wasn’t enough. Her breathing was very laboured. If she twitched a finger, she would get into trouble with her blood-oxygen saturation. Her gut was shutting down and she was getting a build-up of fluids in her lungs and body tissues. The nurses kept her heavily sedated to limit how much Hailey moved.
Monday afternoon also brought another problem with Hailey’s central line – they thought that it was partially blocked. The blockage was likely from a blood clot forming inside the line, or the line migrated and the end was pushed against the wall of the vein. So again, it was a little urgent to get it running properly (see last week). They tried again to get an IV started in her head. We again learned that the NICU Doctors are not estheticians – they had to shave both sides of Hailey’s head to find an appropriate spot for the IV. She now looks like she has a mohawk and a mullet – maybe she’ll start a new fad. On Tuesday, the Neonatologist ordered a dose of Lasix (a diuretic) to reduce the fluids that she was retaining in her body. She also ordered that Hailey be put back on Ventolin, and be given it more frequently and in higher doses than previously. By late Tuesday afternoon, Hailey’s oxygen requirements were way down and her breathing was more relaxed. We were a long way from being out of the woods, but at least she took a step back from the proverbial precipice (excuse the metaphors). On Wednesday evening, Janet’s brother Brad and his family (from Victoria) came to visit Hailey. She was awake enough to give them a wave “hello”. For the rest of the week, Hailey got a little better each day. By Thursday evening (Christmas Eve), Hailey was feeling well enough that she thought that she would extubate herself. Her nurse was looking over her, when suddenly, she heard Hailey cry – and said “Oh no, you didn’t!!” (…because Hailey can’t cry or make other vocalizations with her ETT in). Given how difficult previous re-intubations had been, this was not at all good. Luckily, a baby was being admitted to the bed next to Hailey’s, so there were extra Nurses, Respiratory Therapists and a Doctor next door. They quickly came to Hailey’s beside and got her re-intubated. Also fortunately, it went in on the first try!! Hailey barely missed a beat. Christmas was hectic, as we spent the day bouncing between visits with Hailey and each of our families. Christmas evening, we opened all the gifts that were left under Hailey’s tree by Santa and her NICU “Aunties”. We got a special gift from Hailey – a couple of the Nurses helped Hailey make molds of her feet. It will be a special keepsake for her mom and dad. |
December 14 - 20, 2009
|
The beginning of the week was fantastic – Hailey’s oxygen requirements were way down (often into the 20’s % FiO2 and seldom above 40% FiO2). She was full of smiles and giggles, and really interactive. But she still had a huge leak from her ETT. They wanted to change it sooner than later as it’s possible for patients to rapidly deteriorate without much notice – so they wanted change it while she was doing good, as opposed to doing it in an emergency. They finally set a day – Thursday at 12:30 (yikes).
A couple of the nurses suggested/hinted that we should get a Christmas tree for Hailey’s bedside – so we did. We bought a small 2’ high tree and some small decorations. It had to be unlit – otherwise, hospital engineering would have to check it out first (who knows what that would entail). On Wednesday evening, we decorated it. We set the tree up on a table so that Hailey could watch us – she couldn’t take eyes off the tree and needless to say we had fun. The tree decorations were a little sparse, so Janet and Hailey continued with the decorating Thursday morning after we bought some more. Hailey and Janet finished with the tree decorating just in time for a special visitor – Santa made a special visit to all the children in Children’s Hospital – stopping long enough for a picture. Promptly at 12:30 the Anaesthesiology team walked in…and a few Respiratory Therapists…and a few doctors and nurses from NICU…while we were “invited” to wait in the parent lounge. Within a few minutes, the same people started to file out - a couple of them stopped to tell us that everything went fantastic and the ETT exchange went without any problems. They gave Hailey enough drugs to put down a small elephant though – so she was in “la la land” for the rest of the day…and night. We were a tad concerned on Friday when we arrived to see that Hailey’s FiO2 (oxygen) was up to 35% (up from 28%). We understood, though, that it would take a little time for Hailey to get used to the full effect of the ventilator (without a leak). A little while ago, we were approached by a couple of the nurses about having a special Christmas party for Hailey. We wanted to wait until Hailey’s ETT exchange was done and she was safe before we made any plans or announced any party plans. On Friday morning, once we determined that Hailey was doing well, we sent an email to our in-town family inviting them to a Christmas party on Sunday afternoon. The plan was for the party to be in a conference room just outside NICU. Hailey would be moved into a smaller bed. Then she, her ventilator and her iNO (gas) would be wheeled down the hall to join the party – a daunting task, but doable. On Saturday afternoon, Hailey’s central line broke – double “yikes” and a few more expletives!! Hailey’s epoprostenol is injected through her central line continuously. They basically have 30 minutes to restart the epoprostenol before Hailey would start to get into serious trouble. They tried several times to start an IV in her head, but no luck. However, they managed to jury-rig a fix for the central line and got the epoprostenol running again – it was only off for about 20 minutes –phewww!! We always think about the “what ifs” (we’ve been doing a lot more of that over the past 7-1/2 months), but this time we had to put it into action. When we arrived on Sunday morning, we learned that Hailey wasn’t having a good morning – her breathing was laboured, her oxygen was up and her blood gases weren’t great – meaning that she couldn’t come to the party – it would be too risky. So instead, the party would go to Hailey. Normally non-sibling children aren’t allowed into NICU, but for Hailey, they made an exception – her younger cousins were allowed to come in and visit Hailey for the first time. Hailey’s bad afternoon continued into the evening. After everyone left, we let Hailey rest and stayed with her into the evening. It was hard watching her have such difficulties breathing – it was a very trying and emotional evening as we worked ourselves into a tizzy as we worried where this was leading. |
December 7 - 13, 2009
|
Compared to the past couple of weeks, Hailey had a really good week – lots of smiles and giggles. She was also acting like a teenager – staying up until the wee hours of the morning, and then sleeping in until after noon.
Over the past several days, Hailey’s had quite a leak from her ETT – air leaking out from her lungs around her ETT and out her mouth. At times, it sounds like she’s purring like a cat. Normally it’s not a concern because the ventilator compensates for it. When the leak gets to the 40% - 50% range is when they start to get concerned. Hailey’s was getting to the 80% ballpark – so we started talking about changing her ETT to a larger size tube. It’s likely caused by her growing, swelling in her throat going down or her trachea getting stretched from the constant pressure from the ventilator – or a combination of any of the three. Normally it’s not a huge problem – except last time she crashed (chest compressions and hand ventilation). So this time we want to take every precaution. We had a meeting with this week’s Attending and Hailey’s pediatrician. It was decided that they would ask Anaesthesiology to come and either do it or participate. Anaesthesiologists are considered airway experts. They’re trained to intubate patients within a couple seconds and they do it every day – that’s why the Attending wanted to bring Anaesthesiology “onboard”. On Thursday, Hailey spiked a fever. Over the past several weeks/couple of months, Hailey’s had quite a few fevers. We’ve written most these off to “teething”. All but one – when she had a urinary tract infection – broke relatively quickly. However, this time it lasted until Sunday. During this period, her heart rate was high – which was alarming. They sent off the usual scads of blood, urine and booger tests – all came back negative. So another mystery fever. On Friday, Hailey turned seven months old. “Aunties” Drinda and Kim made a sign – they had to get creative as the letter supply is getting low. They used upside down “y’s”, “7’s” and “3’s” for “h’s”, “L’s” and “e’s”. And “Auntie” Val made delicious gingerbread cookies awesomely decorated with crowns with Hailey’s name, balloons with “7”, and ballerina slippers. |
November 30 – December 6, 2009
|
Hailey’s oxygen requirements improved through the beginning of the week. When they started her Ventolin last Saturday, she was getting it every four hours – this meant waking her up. On Monday, they decided to change her Ventolin to every six hours. Either coincidentally or because of the Ventolin change, the CO2 in her blood started to creep higher and she showed signs of working harder to breathe. So they threw a few more changes at her. They felt that she was working against her ventilator, so they changed her sedative to one that would still allow her to be interactive but would take away her feelings of being “air hungry”. They also changed her Ventolin to a similar drug called Advair which is only given twice a day instead of eight times a day. It took a few days, but her CO2 got under control. Her oxygen requirements also dropped to a better range.
This week, we had a quite a few discussions about the tracheostomy and how it will change our lives - some for the better and some not so good - we have a difficult decision to make. We also had a few discussions about Hailey’s future and alternative ideas floating around about her prognosis – not necessarily happy discussions. Although we both thought about Hailey’s vulnerability and the possibility of losing her, we hadn’t necessarily discussed it in so many words and with someone else. |
November 23 - 29, 2009
|
The beginning part of the week was more of the same as last weekend – Hailey’s oxygen requirements kept increasing and she kept looking more and more uncomfortable. On Monday afternoon, Hailey had another one of her “deep desat. and heart rate drop” episodes – this time while she was being suctioned. Her heart rate and blood saturation levels dropped, she turned grey and unresponsive – while everyone around her, especially Janet, was white as a ghost and scared shitless. The nurses, RT’s and doctors jumped in did what they’re supposed to do – that’s why Hailey is still in NICU (and we’re glad for that).
On Tuesday mornings, the Attending Neonatologist and Fellows do “teaching rounds”. They take turns presenting cases, and teach each other what they’ve learned and discuss alternative solutions. This week, they discussed Hailey. They invited other “ologies” (cardiology, respirology, nephrology and endocrinology) and Hailey’s pediatrician to come and “brainstorm”. Nephrology wanted to do another ultrasound of her kidneys to confirm her renal status. Cardiology wanted to increase her nitric oxide (iNO) to 20 part per million (ppm) and to keep it on for at least another 3 weeks – a total of six weeks after her heart cath – apparently it takes at least 6 weeks for most patients to respond to iNO. For some time, we’ve been asking for a “primary Attending Neonatologist” – as it stands now, the Attending Neonatologists rotate in for a week (some call it “the flavour of the week”). We want to increase the “long term memory” – when an Attending rotates in, the incoming Neonatologist receives each patient’s history (up to 17 patients) for the prior week plus some of the pertinent history from the previous weeks from the outgoing Neonatologist. However, it’s not possible to pass along every nuance of each patient from every single week – in Hailey’s case, that’s many, many weeks. So what we want is for the “primary Neonatologist” to serve as the “long term memory” – each week’s Neonatologist would still be in charge of the acute care (day to day), but Hailey’s “primary Neonatologist” would be there as a guide to what has been done and what has or hasn’t worked. However, we’re told that primary Neonatologists haven’t worked in the past. So what this rather lengthy babble leads to…on Tuesday we reached a bit of a compromise. We were granted a “primary Fellow” for at least a month (while he’s on service in NICU) – so whenever he is in, he’ll be assigned to Hailey. But the whole “primary” thing is becoming a bit of a moot point – most of the Attendings, Fellows and many of the Nurses know Hailey so well because she’s been there for so long. Also on Tuesday, Dr. Seshia (an Attending Neonatologist) discussed with Janet the possibility of doing a tracheostomy on Hailey. A tracheostomy would replace her ETT and would give Hailey more freedom while she’s on a ventilator (possibly for some time – months or years?). It would also be more secure than an ETT – she wouldn’t be able to pick the tape off and there would be less risk of accidentally extubating herself. They don’t make these decisions lightly. There is a panel that reviews each case. It also stands to reason that this is not something that we should take lightly. It may not happen immediately, but it likely won’t be too far in the future. On Tuesday evening, she did it again – she had another episode. This time while she was upset after being weighed. Also, this time they needed to do chest compressions – not something a mother wants to watch happen to her daughter (Colin was curling that night and wasn’t there). Although she recovered in a relatively short period of time, it is still a very difficult thing to watch. By Thursday evening, we, the Doctors and the Nurses were quite nervous. All week, Hailey’s oxygen requirements kept creeping up and her comfort level kept getting worse and worse. Then… If we thought that the day of her heart catheterization was “the biggest and scariest so far”, well…meet Mr. Friday. Through Thursday night and Friday morning, Hailey deteriorated. Her night nurse called us Friday morning at 7:00 a.m. to give us an update – just so that we were prepared when we came in. Hailey’s oxygen requirements were way up – to 80% (up from the previous evenings 50%ish and up from her normal 30%ish), her breathing was very laboured (even more than earlier in the week), her tummy became distended and started leaking feed out her stoma (so they stopped feeding her), and her blood sugar spiked (likely a stress response). All bad things. To say that Hailey was peering over the edge of precipice is not an exaggeration. She was in a very grave position. The Doctors and Nurses, obviously did everything they could to stabilize her condition. They also had many meetings and consultations to figure out their next plans. They figured that her pulmonary hypertension was getting worse and that if we waited 3 weeks for her iNO to catch up, Hailey wouldn’t be with us. They tried a bunch of different things to see if they could figure out what was going on. One thought was that her ETT might have been occluded. So they changed the ETT- but that didn’t go so good. They had trouble reintubating her – so much that Hailey’s blood saturation and heart rate dropped and they needed to hand ventilate her and do some chest compressions. They also did a heart echo. Although it wasn’t Hailey’s worst echo, it was worse than the one that they did a month or so earlier. They also did a renal ultrasound – surprisingly, it was the only bright spot of the whole week. On Tuesday, the ultrasound they did showed that she had almost total blockage to both of her kidneys. She was still producing urine at her normal rate, so they started to question the validity of the ultrasound results. So on Friday, they brought in a bigger, higher-tech ultrasound machine. Apparently it was a quite a big deal to bring it in to the NICU – normally patients go to it. This time it showed normal blood flow to both kidneys (yeah!). However, Hailey was still in much distress… After much debate and consultation, they decided to start Hailey on a new drug called epoprostenol - it’s a powerful vasodilator (it lowers the blood pressure by dilating the blood vessels). It’s so powerful that they have to closely monitor the blood pressure as they slowly increase the epoprostenol dose (over several days). In Hailey’s case, they inserted a line into an artery (an art line) in one of her legs (actually her left foot). Through the art line, they monitor her blood pressure second by second. She seemed to respond to the new drug almost immediately – her blood pressure was slightly better and her breathing seemed to be very slightly less laboured. So we left Friday night with a lump of uncertainty in our throats, but with the knowledge that she was in good hands. Over the past several days/weeks, several nurses have noticed tightness in Hailey’s lungs. So on Saturday, the Attending wanted to try something – an asthmatic drug called Ventolin (a bronchial dilator). It’s difficult to give to someone on a ventilator – so they had to experiment with a couple different delivery techniques. It seemed to work – by Saturday evening, they noticed some decrease in her wheezing and by Sunday, significantly less wheezing. Also by Sunday, her breathing was considerably less laboured and her oxygen requirements were down (to the 50’s %ish). |
November 16 – 22, 2009
|
Monday, was kinda weird – Hailey was awake ALL day and her heart rate was really high. She wasn’t upset – just awake. At some point, she was given a pretty heavy sedative, called Lorazepam, but she just shrugged it off – she just got glassy eyed and never fell asleep (until later in the evening).
The rest of the week : no big changes – just chillin’. Except… Saturday and Sunday weren’t great. She was showing signs of having trouble breathing and needed more and more oxygen. To us, it seemed to be more “mechanical” – it seemed to really depend which way she was facing and how her head was positioned. When the nurses turned her to lay on her other side, she seemed to be more relaxed. But soon, she would start getting into trouble again. |
November 9 – 15, 2009
|
Monday was a big scary day - one of the biggest and scariest so far. Hailey’s heart catheterization was scheduled for 11:00 Monday morning. Colin skipped out of work for the day, so we both got to the hospital early. We had “ants in our pants” as her nurse was getting her ready and until she was taken down (we were a tad nervous). The fact that the cath-lab was late calling her down didn’t help. At 12:30, Hailey’s entourage took her down – Hailey’s nurse Catherine, a Doctor, 2 RT’s, and Janet and Colin. From NICU, we took one of the Children’s Hospital elevators down to the tunnels below HSC, through the tunnels to the main bank of elevators of the General Hospital and through the main corridor to the cath-lab (this kinda sounds like the Berenstain Bears “Bears in the Night”). It was almost comical to see the look on people’s faces as we took this tiny little baby in a giant crib though corridor in an adult hospital.
They didn’t really get started until about 1:30 p.m. We were allowed to go into the cath-lab to give her a kiss and wish her luck. Then we waited... Just outside the cath-lab, there was a small waiting area . We were told that catheterization could take anywhere from 2 to 5 hours – all depending on how easily they could access the vein and artery in her leg. We kept ourselves busy by catching up on previous weeks of Hailey’s blog. Catherine kept coming out and giving us updates – everything was going fine. At one point, we heard cheers when they got into the vein. Then at 3:40 p.m., they were done. Dr. Pepelassis came out and gave us a summary. It all went well – everything looked normal with her heart and the pulmonary bed (the larger pulmonary arteries and its branches thatlead to the lungs). Normally they have to get into an artery in the groin as well, but in Hailey’s case, they used her PDA (read more about it here) to their advantage – they were able “drive” the catheter through the PDA and see the “vein” side of the heart. The other good news was that she responded to iNO (nitric oxide) – meaning that her pulmonary pressures decreased when they introduced iNO and that she should respond to various other types of drugs. Needless to say, by the time we got back to NICU, Hailey was wasted…and so were we. Wednesday was Hailey’s 6th month birthday. She now weighs 2.70 kg…double her birth weight and with a little rounding, 6 pounds!! “Auntie” Drinda made her 6 month birthday sign that says “Hailey is 6 months old – November 11, 2009” and has a cute picture of a dachshund on it. The rest of the week was spent just chillin’ – although Janet went to Minneapolis for an extended weekend of shopping (she left on Friday afternoon and back Monday afternoon) – so Colin and Hailey ate Cheerios and Kraft Dinner and didn’t get dressed all weekend. |
November 2 – 8, 2009
|
Monday was another weird day – another fever and increased heart rate. They opted not to do any blood work though because it only lasted for a relatively short period of time.
On Wednesday we got word that her heart cath was scheduled for next Monday (November 9th). We just had to pray that she didn’t spike another fever between now and then. Thursday evening, Hailey decided that the week had been a tad boring thus far – when we got in that evening, her night nurse, “Auntie” Drinda, was weighing her. Hailey was fine and back on her bed, then suddenly, she turned grey and became unresponsive. Drinda quickly called for assistance and started hand ventilating her – she didn’t need to perform CPR, but we don’t think she was far from it. As quickly as it happened, Hailey recovered. As for her parents and Drinda – we’re still having heart palpitations. No one is quite sure what caused Hailey to do this – it might have been a mucus (booger) plug in her ETT. There is also a nerve that runs down the back of the throat that, when touched the wrong way (by something like the ETT), can cause the heart to stop beating momentarily. Either way, Hailey seemed to recover quite quickly, but the look of her at that moment will be burned into our memories – we never want to see that again!! On Friday afternoon, in preparation for Monday’s heart catheterization, they needed to give Hailey a blood transfusion. Whether related to the transfusion or to Thursday’s “incident”, Hailey started to have some “crazy” high blood pressures – so high that they need to give her a couple doses of a medication to help lower it. It was a tad scary, but the medications helped get the hypertension under control. On a happier note…two of Hailey’s front bottom teeth started to show! Over the past few weeks, Hailey has been having some odd, relatively short low grade fevers and she’s been putting her hands to her mouth very frequently – signs that she’s teething. Well, on Friday evening, we saw two little white streaks poking through her bottom gums. Now her little gummy grin will have some bling!! Saturday and Sunday were ordered “chill-out” days. The NICU attending doctor basically ordered that we and the nurses do nothing with Hailey - i.e., no baths, no picking up, no big tricks – just chilling out until her heart cath on Monday. Of course this didn’t mean that we couldn’t be with her and give little bedside cuddles and kisses – just nothing that would “deplete her reserves”. |
October 26 – November 1, 2009
|
Compared to last week, this week was pretty tame – just one day with a fever and except for…
Part way through Monday morning, Dr. Caces (this week’s Attending Doctor) came to Hailey’s bedside and said “You need to sit down. We need to talk”. Needless to say, that scared the “bejeebers” out of Janet. Dr. Caces told Janet that the Cardiologists (in Winnipeg and Edmonton) wanted Hailey to have a chest CT scan done before the heart catheterization. The chest CT scan can’t be done in Winnipeg, so that meant that she would need to go to Edmonton…and soon, because they want to do the heart cath sooner than later. By this point, Dr. Caces had already talked with the Edmonton Hospital about a bed for Hailey. As soon as a bed was open, Hailey would be on her way…possibly today…tomorrow…Wednesday. Our minds started racing about everything that we needed to do before we left – packing, travel arrangements, hotel, sitter for Higgins, someone to look in on Sedona, etc., etc…that was at about 10:00 in the morning… a little later, at about 1:00 in the afternoon, Dr. Caces told Janet that Edmonton was off. Edmonton wanted Hailey to be off her antibiotics prior to coming (at least 2 weeks away and after her scheduled heart cath). So all of the worry and panic was for nothing…or at least it was a practice run..and got us to think about what is needed to be done for when/if we do go. Edmonton is still on the radar, but a little further down the road. The roller coaster ride called “NICU” continues… On Wednesday, Hailey was quite agitated – they thought it might be Hailey fighting her ventilator. Until now, the vent was set to do most of the work. So they changed it to a different mode where Hailey triggers all of the breaths, and the vent just delivers the correct volume. Thursday was this week’s day with the fever. At about lunch time, Hailey’s breathing started to get more labored (even though she was on the vent), her heart rate started to climb (over 200 beats per minute), and her temperature was up. Still – no idea why. Blood work yet again, and they changed her ventilator settings back to where it does all of the work. The NICU attending doctor was tossing around the idea that it could be a fungal infection – often when people (not just babies) are given antibiotics, the normal (good) “bugs” are killed off with the (bad) ones causing the infection. This leaves room for other “bugs” (fungus, etc.) to move in. They didn’t want to just assume that it was a fungal infection and treat her for it – the treatment can be quite toxic to the kidneys (hers are already compromised - so it is a little risky). We also know that she’s teething. On some X-Ray’s, we can see some teeth – even though they haven’t broken though the surface - plus Hailey’s been putting her hands in her mouth a lot more frequently over the past several days. By Thursday evening, her fever was gone and her heart rate returned to normal. Saturday (Halloween day), when we got in, one of the nurses asked us to wait… when they “let” us in, Hailey was dressed up in a pumpkin toque, Halloween socks, and a “onesie” with “I want my MUMMY” on it. To say she looked adorable was an understatement!! After lots of pictures and lots of “oh, dang she’s cute” from the nurses and her parents, we dressed her in a flower costume that we bought for her – even though it was a 0 to 3 month size, it was WAY too big for her. It looked like a flower was trying to eat Hailey!!! On Sunday Hailey did some “tummy time” for the first time – at first she complained, but then settled down and really enjoyed it. She even fell asleep. Her nurse had made a roll out of some blankets, then propped Hailey up on her knees in the roll with chin resting on her hands on top of the roll. |
October 19 - 25, 2009
|
Early Monday morning, a lab result came back confirming that Hailey had a urinary tract infection (UTI). Hailey’s heart cath was scheduled for about 2:00 in the afternoon – but, due to her UTI, it was cancelled. They can’t risk spreading the infection when they insert and manipulate the heart catheter. In a way it was a relief. It was also a relief knowing that it was a UTI – it was an answer. We couldn’t open up the isolation quite yet – we didn’t have the H1N1 test result yet.
A little later in the morning, we had a meeting with Dr. Seshia (the NICU Attending), Dr. Pepelassis from Cardiology and Dr. Al-Somali from Respirology to determine our next steps. Dr. P had some recent discussions with a Cardiologist in Edmonton. The Edmonton Cardiologist suggested that a chest CT Scan might be valuable and shed some light on Hailey’s anatomy, and could be considered a first step to figuring out what’s going on. We had some discussions of where the chest CT should/could be done – was Winnipeg’s equipment good enough? Was there enough experience with the Winnipeg operators? There were also questions about what kind of information can be gained from the scan – i.e would they be able to get enough detail of the pulmonary vasculature of the lungs? Just after our meeting, we got word that she could come out of isolation – out of the “bubble” as it is affectionately known as. That was a relief – now we didn’t have to get “all dressed” up and we could touch and kiss her. Tuesday was another big day – since the weekend, the nurses and docs were getting concerned about how much urine Hailey was making. They ordered an ultrasound of her kidneys. It took some time to get the results, but it wasn’t great. The blood flow to one of Hailey’s kidney’s, her right one, was almost completely blocked. The flow to left side is great. Having one kidney isn’t a big deal – a lot of people have just one functioning kidney and don’t even know about it. The down side is that when an “unhealthy” kidney is still in the body, the kidneys release a hormone that raises the blood pressure in an attempt to increase the blood flow through the “bad” kidney. Hailey has always had high blood pressure – so now, we’ll have to keep an even closer eye on it. They’re not sure what caused the blockage or even how long it’s been there – it may have been just when she got sick (last Saturday), during her pulmonary hypertensive crisis (early August), or since her birth. We had a meeting with a team from Nephrology, and they recommended not doing anything at this point - they will follow her closely for the foreseeable future. Wednesday… oh ya, another big day!!! When Janet got in, she was greeted with a sign that read “Hailey’s Headquarters This Way” (and an arrow) – Hailey was moved back to her old spot – yeah!!! Also, for some time, they’ve been talking about needing to put in a central line for IV access – a central line is a small surgical procedure where a catheter is inserted in the groin (usually), then fed up a major vein until it’s almost to the heart. The past couple of times that Hailey has needed an IV, they have had GREAT difficulties trying to get one in – often needing to poke her many, many times. In children Hailey’s size, normal IV’s (in the arm, leg or scalp) usually only last for a couple of days. Since Monday, and her UTI diagnosis, she’ll need an IV for at least 3 weeks. Then if her heart cath is re-scheduled, she’ll need it for even longer. So that makes it almost necessary for a central line. So on Wednesday afternoon, after great debate over where it should go, the central line was put into one of her leg veins (femoral) (near the groin). Cardiology wanted to preserve both femoral veins for the heart cath, but the surgeon wasn’t sure if he would be able use any other sites for the central line. On Friday Hailey gave her nurse a heart attack – Hailey decided that it was time to re-tape her vent tube (endotracheal tube, ETT) and ripped the tape (that holds the ETT in place) off her cheek and was just holding it in her hand – luckily, she didn’t pull her ETT out!! Sunday greeted us with another fever…it was quite mysterious. Since last weekend, she’s been on a multitude of antibiotics – so to think that this was another bacterial infection was a little bizarre. But what else could cause it? Teething? A virus? We/they’re not sure, but they did more blood work, etc. to find out. By Sunday evening, the fever was gone, and she was more comfortable. |
October 12 - 18, 2009
|
On Monday (Thanksgiving Day), Hailey had a good day. Although, later in the afternoon, her nurse noticed that she needed an increasing amount of FiO2 (oxygen), so they did another X-Ray. The neonatologist fellow noticed that she continued to have some wetness on her lungs (it looks hazy on X-Ray) and her heart is slightly enlarged – meaning that it’s having to work a little harder – so he ordered another round of Lasix to reduce the fluids that she’s retaining in her body.
Tuesday and Wednesday, Hailey was alert, active and comfortable, but she needed increasing amounts of FiO2. By Thursday, her FiO2 was considerably up and her breathing was becoming noticeably laboured. She puzzled everyone – her X-Rays looked unchanged since the weekend and her demeanor was good. Thursday morning, Dr. Pepelassis from Cardiology came to do another cardiac echo – since her last echo (at the beginning of September that looked great), this one didn’t look as good. He noticed an increased flattening of her septum and some slight regurgitation (meaning that the PPHN is more noticeable then it was at the beginning of September). Also, a blood test showed that her hemoglobin was slightly low (hemoglobin helps transport oxygen from the lungs to the rest of the body) and her reticulocyte count was low (“retic” is a number that indicates how much new blood the body is making). At the beginning of the week we requested a “team meeting” to discuss where we’re at and what our plan was. The meeting was scheduled for Thursday at noon. In all, there were 12 of us (the NICU Attending, a fellow and nurse; 2 from Respirology; 2 from Cardiology; 2 from Symptom Management/Anaesthesiology; 1 from Respiratory Therapy; plus Janet and Colin). Our main focus was Cardiology and Respirology – but Cardiology and talks of the cardiac catheterization (“heart cath”) seemed to monopolize the discussions. Earlier (see June 22 - 28, 2009), we talked about doing a heart cath to help determine what might be causing Hailey’s PPHN and how she might respond to different drugs and treatments. Shortly after those discussions, we started her on Sildenafil – which she seemed to respond to – so the heart cath got deferred until she was at a much safer weight because it would be more of an investigative procedure than a diagnosis for treatment. …but now that Hailey’s PPHN appears to have reared its ugly head again, we’ve had to re-open the heart cath discussions. The Cardiology team wants to determine the “real” pressures in her heart (opposed to “guessing” from a heart echo). By getting the real pressures, they would be able to determine what drugs they can use and at what doses. They can also use the heart cath to help them see the heart’s and pulmonary system’s anatomy. During the team meeting, Dr. Pepelassis told us that the cath lab had an opening on November 10th. They also reiterated some of the risks involved with doing a heart cath. Although everybody kept telling us that the decision is entirely ours – we still got the feeling that this is our only logical course. They asked that we take all the time that we need and let them know. But… Very shortly (minutes) after our meeting finished, Dr. Pepelassis called the NICU – they had an opening in the cath lab this Monday!!! Same rules applied…the decision was entirely ours. He asked that we think about it and let them know sometime Sunday. On Sunday, they would need to intubate her and do some blood work. If, on Monday, we didn’t feel comfortable; no questions, we could cancel. The upside is that there would be doctor in from Edmonton that would be assisting Dr. Pepelassis. Later Thursday night we talked about the heart cath. We both agreed that it was our only course of action and felt like the right thing to do. Friday met us with another slide in Hailey’s condition. The NICU docs wanted to start a blood transfusion to see if it would help (as mentioned above, her hemoglobin and retic counts were low). They started the transfusion at about 2:00 in the afternoon. Shortly after, she started to get very agitated and her breathing became very laboured. They stopped the transfusion thinking that the extra fluids in her system were overloading her. By the time Janet got home late Friday afternoon, the NICU Attending Doctor called Janet to let us know that Hailey would need to be intubated… By the time Colin got home (a little more than 5 minutes later), the attending called again to tell us that the intubation went very well (first try) and that she seem more comfortable already. On Saturday, when we got into the NICU, we were told that Hailey started a fever earlier that morning, and, as a result, they sent blood and urine samples, and nasal and throat secretion swabs to the lab to check for infections. On Saturday evening, we got an odd call from Hailey’s night nurse – because of the swabs that they sent and the simple fact that they asked for the H1N1 Influenza to be checked, according to hospital policy, Hailey had to be moved into isolation (still in NICU, just a few beds over). So that evening (and for the foreseeable future), Hailey’s bed was behind a thick plastic curtain – to call it isolation is quite a stretch considering that there are gaps at the top and bottom of the curtain and there is an air vent blowing air into the curtained off area. To get into see Hailey, we had to put on a gown, gloves, eye shields and a respirator (a.k.a. mask) – we kinda looked like yellow Darth Vaders. Sunday was not a good day – we had enough. To say we both had an emotional breakdown is a tad of an understatement - to cry with eye shields on and get “snotty” noses with a respirator on – not a pretty sight. Between Hailey being sick, Hailey in isolation (mostly us not being able to hold her the same as without the “isolation garb” on) and the stress/fear/anxiety of the hearth cath likely pushed us over the top – if any one of those 3 “stressors” were not in the picture, we likely would have been OK. But we both admit that it was good to get it out. |
October 5 - 11, 2009
|
Hailey was on CPAP for all of last weekend and had a really good Sunday night and Monday morning. The docs decided to do nothing and give her another day on CPAP. This was a good thing. However, Tuesday was a bit of a test – they were going to try Hailey off of CPAP for a few hours. She seemed stressed while she was off of it. She was back on CPAP, as planned, for the night. The plan going into the week was that we would try her off CPAP during the day for increasing blocks of time. After seeing her reaction on Tuesday and after consulting with Respirology, the docs decided to keep her on CPAP for a few days - if not a few weeks. They feel that her lungs may need some time to heal and grow.
Wednesday was a good day. Janet’s Auntie Linda and Cousin Matt were in from Kelowna and came by NICU for a visit. Hailey “hammed” it up from them. That night, Janet had a “girls night out”, so Colin did a solo bath night with Hailey – both behaved themselves, but nurse “Auntie” Cathy had to step in a few times to break up some water fights. Last week, Hailey’s “feed” was changed from a pre-mixed version of Pregestimil to a higher calorie powdered version that is mixed with water at the hospital. Through the week, Hailey started gaining weight. By the end of the week, she gained 120 grams (4.2 ounces). This is the first significant weight gain since the end of July – we’re not keen on seeing her gain a lot of weight (see July 20 - July 26, 2009), but agree with the docs that she is needing to gain some weight to help her grow. She’s still not liking bath time. We joke that she has Child and Family Services on speed dial and reports us – “They’re given me a bath – AGAIN!!!!” On Saturday morning, Hailey was tachypneic (breathing faster than normal), diaphoretic (sweaty) and had a slight increase in her FiO2 requirements (oxygen), so they suspected something “was up”. So they did an X-Ray and it showed some wetness in her lungs (it looks hazy on X-Ray). They gave her a dose of Lasix (a diuretic – makes you pee – a lot!!), thinking that she had some excess fluid hanging around – mainly due to her significant weight gain over the past week. On Sunday, she was doing better, but they felt that she needed another dose of Lasix to “dry” her up a bit more. Later Sunday afternoon, they did some blood tests to check her gas levels (O2, CO2 and Ph) and her electrolytes and another X-Ray. The blood work came back good, and the X-Ray showed some improvement since Saturday. Sunday was also Hailey’s fifth month birthday!! Nurse "Auntie" Kim celebrated by making a sign for her bedside that read “No Bats About It, U R Boorific. Hailey’s 5 Months Old on October 11th” (Halloween theme, of course). |
September 28 – October 4, 2009
|
On Monday, Doris (the clinical nurse from NICU) took us for a tour of PSCU and “the ward”. The Pediatric Special Care Unit (PSCU) is a longer term care unit that would fit in somewhere between an intensive care unit (NICU or PICU) and a regular ward. The patients are still heavily monitored and the nursing ratio is still pretty high (1:1 or 2:1 – similar to NICU). They are able to focus more on the developmental needs of kids and on their chronic health care needs (opposed to the more reactive acute care of NICU). Later in the week, it was decided that Hailey is a good candidate for PSCU, but not immediately - she still requires too much attention. They will re-assess her in a few weeks to see how she is doing. If she’s ready and if they have a bed open, they may consider her again.
On Monday afternoon, Hailey’s feed was switched from breast milk to a bottled formula called Pregestimil. That evening she had her first “formed” stool – yeah, yeah, we know, another poop reference. On Monday evening, Hailey had her first “real” bath since her GT surgery – although she didn’t enjoy it, she got to splash around and soak in the tub for a few minutes. Late Tuesday afternoon, they tried her off CPAP – she didn’t like it at first but she settled down after a few minutes. She got all the nurses excited – she had “formed poops” all day Tuesday – we know it sounds kinda weird, but she’s never had anything but “liquid poops”. This could explain some of the irritability – maybe (and obviously by looking at it) her butt hurts? Maybe she gets stomach cramps? Maybe this Pregestimil is working for her? Time will tell. Again, Wednesday was a good day - on CPAP last night but off during day. Through Wednesday night her GT developed a crack in the top (where they connect it to Hailey’s feeding syringes). It had to be replaced. Sounds straight forward, but a surgery fellow had to come and put the new one in, then there was doubt that it was in her stomach – but an X-Ray answered that (all was OK). She had a really good day and evening with lots of giggles and smiles. So it was decided to keep her off CPAP through Thursday night. Friday – not so good. Hailey’s breathing was becoming very laboured through the morning. She was using lots of accessory muscles to breath (i.e., using her shoulders and drawing in her tummy). They checked her blood gases – she was in big trouble – her CO2 was through the roof, Ph was way off. So they immediately put her back on CPAP. They told us later that she was within a whisker of needing to be intubated. For the rest of the weekend, we pretty much let her chill out and relax – on CPAP. |
September 21 - 27, 2009
|
Hailey was still very irritable. She seemed to calm down when being held. We’re not sure if this is health related (PPHN? Stomach?), or simply that she’s 4-1/2 months old and has figured out that if she raises a fuss she’ll get a cuddle. We’re worried about letting her work it out herself - it’s possible that if she gets too upset, it could lead to another setback. When she was being held, she was quite “talkative” (cooing and making cute baby sounds), and had many smiles and giggles. It definitely brought smiles to our faces and tears to our eyes!
Hailey went on a “road trip” on Wednesday evening. Nurse “Aunties” Drinda and Cathy got a portable oxygen bottle, and we packed up Hailey’s “supper” and oximeter. Then the 4 of us trotted across NICU to the bonding room to surprise Janet - who was in there pumping (getting more milk for Hailey). Needless to say, Janet was pleasantly surprised to find Hailey and Colin knocking at the door. After Janet was finished, we completed our tour, by going to visit all the other NICU modules. On Thursday, Hailey woke up very irritable and wouldn’t settle. Her heart rate was very high and her breathing was very laboured, so they decided to put her back on CPAP. She seemed to settle down right after going back on. They thought she would only be on it for a few hours, but when they tried to take her off later in the afternoon, she became agitated again and desaturated quite dramatically. So back onto CPAP she went! Early Thursday afternoon, we met with Dr. Seifert (Clinical Pharmacist) and Dr. Seshia (NICU Attending) about starting a new medication to help calm Hailey. We discussed a number of options, but a drug called Clonidine seemed to be the most logical starting point. At the doses that Hailey will get (extremely low), it helps block some of the anxiety that causes her to get so worked up. A side effect, like the Sildenafil, is that it lowers the systemic blood pressure – for her, that’s a good thing. They’ll keep a close eye on her blood pressure – we don’t want it getting too low. On Thursday, we also met with Dr. Moroz (Gastroenterologist) to see if he had any thoughts on why Hailey keeps having the water loss stools (which she has had from day 1). He thinks that she might be lactose intolerant, so they have started adding Lactaid drops to her milk to see if this will help. We’ll try it for a few days to see what it does (keeping our fingers crossed!). Thursday evening and through the weekend, she remained on CPAP. She got lots of cuddles with her mom and dad. On Saturday afternoon, Colin and Hailey ”giggled their pants off” – Colin’s eye’s got leaky from all the smiles from Hailey. |
September 14 - 20, 2009
|
This was a very frustrating week – not knowing what was going on with Hailey’s stomach and why she was so inconsolable at times.
Hailey continued to have lots of “water loss” stools. On Monday morning it appeared that she wasn’t digesting any of her food – sounds kinda gross, but the stuff coming out the bottom end looked pretty grayish-white. Yeah, yeah…we know, we said that we weren’t going to tell stories about every pee or poop, but we felt that this merits an exception!! It was decided to stop her feeds for a couple of days to give her tummy a chance to recuperate. She continued to be extremely fussy and appeared to be in a lot of discomfort. Her stomach was also quite distended. So, on Tuesday, Dr. Wiseman decided to remove the remainder of the water from the balloon at the end of her GT (the balloon helps hold it in). He thought that the balloon might be interfering with stuff getting out of her stomach and that the sutures should hold the tube in, but…< On Wednesday morning “Auntie” Sandra felt her heart in her throat as she discovered that Hailey’s GT fell out!!! So we spent a few anxious hours waiting for Dr. Wiseman to come and look at it. When he finally came, he was casually holding an oral feeding tube and talking with us – we figured that he was just holding it to see if it was an appropriate size. The next thing we knew, he stuck it in her stoma. That caught us off guard, as we were expecting some big sterile procedure. After he “shoved” it in, he wanted a couple of x-rays to be done just to confirm that it was in the right spot. The oral tube was then replaced with another, smaller Foley catheter. The upside is that it’s now in the correct spot – in her stomach – yeah!! In the midst of Dr. Wiseman’s visit, the NICU docs were trying to draw blood for some tests to see if they could figure out what was going on with Hailey’s stomach. This involved trying to get a needle into one of Hailey’s small veins – not the easiest thing to do on such a small baby, especially when there is some baby “pudge” to contend with. In all, we counted 6 attempts. Hailey didn’t seem to mind too much - she was given a drug to help her “see pink elephants” instead of feeling like a pin cushion. At some point she even giggled at one of the docs as he was poking her with a needle! Also on Wednesday, Dr. Pepelassis from Cardiology came to do another cardiac echo – everything appeared “pretty normal” – some good news for the week. On Thursday evening, Hailey was having a little trouble breathing. They did a chest x-ray and thought she had a slight collapse of her left lung, as well as some wetness on her right lung. Because of this, she needed to go on CPAP. While trying to rig up a CPAP cap over her IV (which was still in her scalp), her IV came out! We had been hanging onto this IV with our lives (since last Sunday), as she doesn’t really have many more spots to have IV’s put in. So they tried 4 times to get a new IV while we were there, but no luck. Then they tried another 4 times through the night (including one in the scalp that involved another small NICU haircut), but still no luck. Also though the night, in order to keep her blood sugars in the safe range, they started feeding her breast milk through her GT. On Friday, the results from the blood tests came back. Everything was negative, so they didn’t worry about getting another IV in at this point – whew!! Hailey still remained irritable, but none of us could figure out why. On Sunday morning, Hailey woke up quite upset, so they tried taking her off CPAP. It didn’t help much – she was still pretty upset, and at times inconsolable. |
September 7 - 13, 2009
|
This was another scary and challenging week. The Labour Day long weekend was full of talk about Hailey being extubated. The docs felt that Hailey was ready to be extubated before her G-tube surgery (see last week), but since she needed to be intubated and on a ventilator for the surgery, they “dragged their feet” for a couple more days. For a couple of days following the surgery, Hailey needed the vent as she recovered from the effects of the anesthesia – by the beginning of the week, she was ready again. They wanted to have an Ear-Nose-Throat Specialist present to do an endoscope of her trachea as they extubated her. Both at birth and on “Black Thursday”, they had some difficulties intubating her, so they wanted ENT to make sure that there wasn’t anything “funny” going on with the anatomy of her trachea that may have contributed to “back Thursday”. Through the ENT’s intern, NICU tried to arrange the extubation for Tuesday – but no dice. On Tuesday morning we got the word that it would be done on Wednesday at noon.
It was expected that once extubated, Hailey would need to be put on CPAP. So just before noon, Respiratory Therapy brought a CPAP machine to her bed side, as well as other things that they might need. Then the “buzz” began as everyone kept asking when it was going to happen, etc. etc. We then got word that ENT was called into surgery and would be delayed….arrrgggg. Then at just after 12:30 everybody was present and in their places. It was decided that ENT would not do an endoscope as they didn’t feel that it would be necessary and wanted to save Hailey the extra “trauma”. So at 12:40, with very little “fanfare” – just a mere 12 people (including her hyperventilating parents) standing by her bedside and with one last “puff” on the hand ventilator bag, Hailey’s ETT was pulled out. Right away she began to whimper – not cry, just a weak whimper. We weren’t sure what we were feeling – worried, happy, concerned, ecstatic…all of the above…she was breathing on her own…we weren’t though – we were holding our breath!!! Slowly everyone dispersed. Eventually it was just Hailey, us and Sandra (Hailey’s nurse that day)...and after 34 days of being on the ventilator - Hailey was breathing on her own!! It was decided that she didn’t need CPAP (for now) - she would just get some additional oxygen though nasal prongs...like just before “black Thursday”. Sandra wrapped up Hailey for Janet to cuddle with her. It was so nice without having to worry about how her ETT was positioned or if it was being pulled or pushed. Hailey eventually stopped whimpering, and we eventually started breathing. Remarkably, Hailey seemed to breathe easier as she fell asleep. She only needed a little extra oxygen when she got upset (like diaper changes, etc.). She improved with each passing hour. By Friday she was doing really good (still no CPAP), and we began to breathe and sleep a little easier. We even had a meeting on Friday with a nurse from Home Nutrition and talked about the “H” word – home. She started training us on how to deal with Hailey’s G-tube (cleaning, changing, problems, etc.) when we get hhhh...hhhhhho…hhhhome. On Friday, Hailey turned 4 months old!!! Nurse "Auntie" Cathy celebrated by making a sign for her bedside that read “Bugs and Kisses, Hailey Is 4 Months Old Today”. Since “black Thursday” Hailey has been fed “continuously” - meaning that her milk is injected very slowly all day and night. On Friday, “Auntie” Cathy (her nurse that night) noticed that Hailey really wasn’t getting the full amount of milk that she’s supposed to be getting. Over the course of the day her milk would be turned off for short periods of time – for baths, to inject medicine, or to change feed syringes. These short periods would accumulate 30, 45 sometimes as much as 60 minutes. So at rounds on Saturday morning, the docs decided to inject her milk over 3 hours with an hour off (3 on, 1 off all day). This way she should get her full daily amount while still allowing for the short stoppages. Then, either coincidently or because of the change made with her feeding, she started to get “water loss” stools (diarrhea) in the afternoon and continuing through Sunday. She got quite irritable and lethargic. On Sunday, because she was dehydrated, they started an IV to replace some of the fluids that she lost. On Sunday afternoon they sent off a sample of her stool to check if it’s a viral thing or a something else. We were also waiting for a surgical consult from Dr. Wiseman to see if it could be related to her G-tube placement (possible causing an irritation to her duodenum) - for now it just a matter of letting her rest and maintaining her fluids. We’ll keep you posted…next week. |
August 31 - September 6, 2009
|
This was another apprehensive week for us. Weeks ago, long before her crisis, Hailey was scheduled to have a gastrostomy (G-tube) put in on August 31st (Monday). Mysteriously last week, it was rescheduled for the 9th then, mysteriously again, for the 4th. On Tuesday, at about 4:30pm, Janet got a call from one of the nurses – the OR called. They had a cancellation and wanted to do Hailey’s G-tube tomorrow at noon!!
A gastrostomy is where a small hole is made through the skin and abdominal wall and into the stomach (this hole is called a “stoma”). A small tube is then placed through the hole into the stomach. The end of the tube has a small balloon to prevent the tube from being accidentally pulled out. Through this tube is how Hailey will be fed for the next while – most likely for the next 3 or 4 four years. Children with RSS typically struggle with reflux (puking) and a loss of appetite - believed to be directly part of RSS and an aversion to food from the constant refluxing. The G-tube helps reduce (or sometimes, eliminate) the reflux and helps us ensure that she gets an appropriate amount of calories and nourishment. Early Wednesday morning, Hailey’s night nurse (“Auntie” Cathy) had to put in an IV and draw some blood for some pre-op tests. Cathy successfully got an IV into one of Hailey’s feet, but after the blood was drawn off, it stopped working (this often happens). Cathy then got another IV started in Hailey’s head – it sounds weird, but this is a common place in babies. Then, while doing an x-ray, the x-ray technician “accidentally” bumped the IV out while adjusting Hailey’s position. Apparently, Hailey had to restrain Cathy from jumping over her crib to strangle the tech ;-). Cathy decided to leave the IV for Hailey’s day nurse – by this point, Hailey was a tad annoyed. The rest of Wednesday morning was spent making sure that everything and everybody was ready to go. Shortly before noon, Dr. Wiseman (the surgeon), came by for one last examination of Hailey and one last look through her chart. He was shortly followed by the anesthesiologist to do the same, and then, at shortly before 1:00, she was off…with her entourage - the anesthesiologist, an OR nurse, Hailey’s day nurse (Stephanie), and Colin and Janet. In the OR area, we said good bye and good luck, and then we were shown to a waiting room. The NICU docs and nurses told us that they expected it would take about an hour from the time that she was wheeled into the OR. So at 2:00 we started expecting someone to tell us that it was all over…then 2:30…then 2:45…by this time we were “going off the walls”…then, finally, at 3:00 a nurse came in and told us that all went well, and she was on her way back to NICU. We caught up with Hailey and the rest of her entourage in the elevator…this time joined by Dr. Wiseman. On the way up, Dr. Wiseman told us that everything went well, but that he found something a little unusual. He found some old blood in her abdominal cavity and thought that her liver looked a little flattened. This apparently happened while the nurses were giving her CPR during her crisis. We were told that it’s not unusual and told not to be alarmed. An ultrasound would be schedule for Thursday just to make that everything was alright. The rest of the day and evening, Hailey was comfortable, but asleep. Janet’s brother, Brad, was in from Victoria and visited with Hailey during the evening. Thursday was another rough day. Early in the morning, Hailey started gagging and puking pretty regularly. At first they weren’t concerned as this often happens when babies start to recover from the anesthetics used during the surgery. However, it continued into the afternoon. Dr. Wiseman was called for an opinion but wasn’t available (he was in surgery). An intern came by and would report to Dr. Wiseman. All afternoon we waited…nothing. Finally, Dr. Wiseman was able to make it into NICU after his surgery duties were finished (early evening). By this time Hailey’s tummy was quite distended (swollen). Dr. Wiseman asked that an OG tube (a tube down her mouth and into her stomach) be put in. He suspected that there was a buildup of “stuff” in her stomach that wasn’t moving through or allowed to move through (i.e., blocked). They struggled for some time to get it in – normally it’s not an issue, but this time it decided to give them trouble. Once the OG was in, they drew out 20 ml of fluid (stomach juices, etc.) – quite a bit for Hailey. Almost immediately, Hailey began to relax. Dr. Wiseman also reduced the size of the balloon at the end of her G-tube. He suspected that it might be blocking the “exit” of her stomach. On Friday morning, they did an x-ray of Hailey’s stomach to make sure that everything was OK with her G-tube…almost comically, it wasn’t. The G-tube was all the way through her stomach and into her duodenum (the beginning part of the small intestine). Keep in mind that Hailey’s stomach, after a “buffet turkey dinner” is about 54 ml in size (a little more than 3.5 tablespoons) – so it’s easy to understand how easy it would be to push it all the way through the stomach. As the stomach isn’t needed very much to digest breast milk, this shouldn’t be a problem. After her stoma has had a chance to heal (in about 2 weeks), Dr. Wiseman will pull the G-tube back a bit. Also on Friday, they started feeding her again. By Saturday afternoon, she was back on “full feeds” (not supplemented by IV fluids). Saturday and Sunday were really good days. Hailey actually slept through having her stoma dressing changed. |
August 24 - August 30, 2009
|
This was a very apprehensive week for us. On Monday she was scheduled for a cardiac echo. The plan was to keep her iNO at 2 ppm through the weekend, then during the echo, turn it off and see what happens. Our brains knew that she would be closely watched, but our hearts were still quite nervous. She made it through the echo without any trouble and it didn’t show any signs of PPHN.
Later in the week there was talk about us having a meeting with Cardiology on Friday morning followed by them turning off her iNO for good (maybe). This really made us nervous. The last time this happened was the day before “black Thursday”. Everybody tried to reassure us by pointing out the many differences between this time and “black Thursday”: her airway is preserved by already being intubated; the iNO machine will remain beside her bed and could be turned back on in a heartbeat; and, they know what signs to watch for when she is about to have a pulmonary hypertensive crisis. But that didn’t help – we were still on edge. The meeting with Cardiology didn’t happen, but after consultation with the NICU docs, we agreed that it was the right time to give it a try. At 11:20am, Friday morning, her iNO was turned off. She went through the afternoon and evening without missing a beat; her oxygen levels remained the same. However, the last time we were at this stage, she ran into trouble through the wee hours of the morning. So we went home on edge, worrying that our phone would ring at 5:20 in the morning…it didn’t. Saturday morning we went in – she had a good night. Her oxygen levels remained really good all night. She didn’t have any other signs of distress. At 24 hours, we gave a barely audible “yeah”. Then at 48 hours, a little louder “yeah” …we’re far from being out of the woods, but she’s on the right track. |
August 17 - August 23, 2009
|
We and Hailey were more relaxed this week. Hailey was a lot more alert and seemed very comfortable – even though she has a garden hose shoved down her throat.
As would happen with anyone, Hailey’s body is reacting to having a foreign object in the lungs (such as her endotracheal tube, ETT) by producing some secretions. Since Hailey can’t cough the “goobers” out and around her ETT, the nurses have to frequently feed a suction line down the ETT to suck everything out. They tell us that it’s like holding your breath, then having someone sucking that breath out. She panics everytime that they do it, but it’s unavoidable. She seems to hate getting her mouth sucked out even more. On Wednesday, Hailey turned 100 days old!! We celebrated on Friday, by bringing brownies for the nurses and Hailey a "100" balloon. |
August 10 - August 16, 2009
|
Hailey was pretty sedated through the weekend and the early part of the week. On Wednesday, her ventilator was changed from a mode where the machine does all of the work (called A/C+VG) to a mode where Hailey was triggering all of her breaths (called PSV+VG).
Hailey’s Sildenafil dose was also adjusted. Previously her dose was 1.5 mg/kg/dose. Through the week, it was increased to 2.0 mg/kg/dose. Previously she was allowed to grow out of her last dose – meaning that the weight that they used to calculate her dose wasn’t changing to match her actual weight. Her new dose is more per kilogram, plus it matches her actual weight. There is no way to tell for sure, but her smaller dose combined with her growing out of it, may have contributed to her crisis On Tuesday, Hailey turned 3 months old!!! Nurse "Auntie" Cathy celebrated by making a sign for her bedside that read “Flip, Flip, Hooray, Hailey Is 3 Months Old Today”. |
August 3 - August 9, 2009
|
Over the past week Hailey has still gained a lot of weight. So with our encouragement, they dumped the additives and she would get just straight breast milk (EBM). We still want to slow her weight gain so that it better matches her length.
Her iNO continued to be weaned. On Wednesday morning at about 10:30 it was turned off. After lunch the iNO machine was gone. Wednesday was a really awesome day. She had a bath, we changed her bed, daddy and Hailey cuddled…it was nice to be free of the iNO machine and to only have the much smaller oxygen hose and nasal prongs. Then… On Thursday morning, at 5:20am our phone rang…NICU – this can’t be good… At about 4:50am Hailey “crashed”. Her heart rate dropped to 30 (instead of 150), her blood oxygen levels dropped to the 40’s…not good. “Auntie” Cathy (her nurse that night) and “Auntie” Drinda started to perform CPR. It turns out that she had a “pulmonary hypertensive crisis” – meaning that her pulmonary system spasmed and prevented any blood from getting from her heart to her lungs. Then her heart “backed up”, causing it to shut down. All not good things. One good thing is that her PFO (see “June 22-28, 2009”) may have helped save her – that as well as Cathy and Drinda beating on her chest and pumping oxygen into her. The PFO may have “shunted” some of the blood to the other side of the heart, helping to decrease the pulmonary pressure and allowing blood to be pumped through to the rest of her body. The whole thing was over in less than 4 minutes. I’m sure for Cathy and Drinda (and everyone else that came to lend a hand) it seemed like a lifetime. Needless to say, once we got the call we got dressed and made our way to the hospital. Then…as weere walking to the entrance of the hospital, we got a call on Janet’s cell phone – NICU again. Because of the huge “hit” that Hailey’s body had taken, she needed help breathing. They had to intubate her and put her on a ventilator. During a crisis like the one that she had, the body shuts down some organs and puts others into overdrive (an adult would be down for month). The nurses walked us through everything, explaining what had gone on, what her body was doing and what to expect. An IV was started to administer drugs and nourishment. An arterial line was also inserted into her leg to draw off blood samples (to check chemistry and other levels), as well as to keep a constant eye on her blood pressure. Her kidney’s took a massive hit, and “took the rest of the day off”. This caused a lot of the fluids in her body to start to settle into the rest of her tissues. Her face was so puffy that she couldn’t open her eyes (if she were awake enough to do so). She was on pain medication (morphine) and sedatives (midazolam and chloral hydrate) to let her “chill out” for a couple of days. They didn’t want her in any distress as it might set off another crisis. We would later refer to this day as “Black Thursday”. There were also rumours spreading around NICU that “Auntie” Cathy leapt over a rocking chair to save Hailey…she denies this, saying that her “super woman costume” was at the dry cleaners. The rest of the week, we just took day by day. Each day, we hoped for the best but expected the worst. But each day, she showed us that she’s a fighter and showed small improvements. Soon she was opening her eyes – through the puff and all. |
July 27 - August 2, 2009
|
On Monday, we met with Nutrition. We had some trepidation about talking to them – of all the people involved with Hailey’s care, we thought that they would be the most reluctant to reduce her caloric intake. But they were on board and eager to learn what we learned. We decided to decrease the amount of Progestimil that is added to her milk. This should slow her weight gain down until her length can catchup.
A little scary, but they’re talking more about home now. It’s something that both of us have noticed – they never really talk about going home or when. We presume that’s so that they don’t get your hopes up. This week is really the first time that they’ve mentioned “when she’s home”. We had a meeting and talked about what she’ll need at home (oxygen, etc.) and what additional care we might need. For the past several weeks, she’s been requiring increasing amounts of oxygen. After discussions with respirology, it was decided to turn her oxygen fully on. Their thoughts are that it’s better for her to get too much than to keep desatting. With a full term baby, there is little detriment to having too much oxygen. The constant desatting could be bad for her organs and brain. At the end of the week, they started to wean her off of her iNO. By the end of the following week, she should be off it. On Saturday, we asked Father Isidore to came by and Baptise Hailey. It was a short ceremony, but very special time with just Janet, Colin, Father Isidore, and the guest of honour, Hailey. Once Hailey is out of the hospital, we will have a “full” ceremony with our family and friends. |
July 20 - 26, 2009
|
Another cardiac echo was done on Monday. There have been some improvements, but the Sildenafil will take some time to work. However, they increased her Sildenafil dose to 1.5mg/kg/dose every 6 hours.
On Thursday, we left for a MAGIC Foundation conference in Chicago. So Janet spent much of the week getting some of Hailey’s medical history, test results and other information together for us to take. MAGIC (Major Aspects of Growth In Children) is a foundation that covers a number of growth hormone deficiency and other growth disorders – Russell-Silver being one of them. Every year they have a conference in Chicago. It lasts for 4 days and has numerous seminars from medical specialists and plenty of opportunities to network with other RSS families. We see that this may become an annual pilgrimage as it will further educate us about RSS, expand our network of RSS families, and, as Hailey gets older, it will allow her to see and be with other kids that are just like her. Thursday was difficult…this was the first time leaving Hailey. Of course she was in fantastic hands and was well cared for…as with any parent, it was still hard to leave her. In the morning, we dropped Higgins (our dog) off at his obedience trainer to be kenneled for the rest of the week. Then we went to the hospital one last time before heading off to the airport. Shortly after arriving at the hotel, we had a meeting with Dr. Harbinson. Dr. H is an endocrinologist at Mount Sinai Medical Center in New York City. She has over 150 RRS patients and has been heavily involved with MAGIC. Every new MAGIC family is offered a complimentary consultation with Dr. H. Normally she will examine the baby, but since Hailey was still in NICU, that was impossible. Instead, they asked us to bring pictures of Hailey. We were in the room with Dr. H for maybe 8 seconds and she had a picture of Hailey for about 1.5 seconds, and she said “Your baby is too fat. They are over feeding her.” She also said the RSS babies shouldn’t have too much subcutaneous fat (fat under the skin) and that you shouldn’t be able to see rings and rolls of fat. RSS children can become insulin resistant very quickly - that can lead to a whole mess of problems. Needless to say, we were a little dumbfounded. Sometime later we looked into what she meant. Most growth charts (that every parent looks at) compare a child’s weight to their age. There also charts that compare a child’s height (or length) to their age. On both of these charts, Hailey is well below the 3rd percentile. However, when we looked at a chart that compares her length to her weight, she was near the 95th percentile…meaning she is much too heavy for her length. Later in the weekend we had another discussion with Dr. H and asked her for some advice on how to broach the subject with the medical professionals at home…like all of us, they have egos too, and we had concerns that we wouldn’t be listened to. The rest of the conference was fantastic. A lot of it dealt with growth hormones – we won’t have to worry about that for a couple of years (when Hailey’s about 2 years old). As well there was a lot on feeding and nutrition – that’s a little closer, but it’s hard when we don’t know what feeding issues she might have (if any) – other than immediately because of her cleft palate. We also met a few family’s that have children with RSS, including 2 from Manitoba. It turns out that there are 5 Manitoba families with RSS children – the oldest is 13 years-old and Hailey is the youngest. While in Chicago, we also got a chance to meet up with friends from Winnipeg and do some sight-seeing – although it was nice to be away from the routine of going to NICU, we were very eager to get home to see out little peanut. |
July 13 - 19, 2009
|
The week was an incredibly sad week…friends that we met through NICU, Shauna and Chico, lost their son Matteo Monday night. Matteo was in NICU for 98 days, and then suddenly passed away after being at home for just 12 days. We didn’t get to know Shauna and Chico very well – not much more than just “hi” and “bye” in the unit. Janet and Sauna had “Wednesday Coffee” together…and we only briefly got to meet Matteo in the unit. For both of us, Matteo’s funeral (on Saturday) was one of the most difficult things that we’ve had to do. We can’t even imagine, nor can anyone imagine what it must be like for Shauna and Chico. As parents of a young baby in NICU, we can only empathise with how precarious the life of a NICU baby can be. Our hearts go out to both of them.
On a happier note; On Sunday night Hailey moved to a big girl bed – she’s now in a crib!! She also changed “rooms”. She still has a window seat – bed number 11 in Module C. The crib is so big that we loose her in it! At least it gives us more room spread out her toys and other things that we use to entertain her. On Tuesday Hailey had her 2 month vaccines – 2 of them in her poor little (chubby) thighs. Editor’s note: Hailey was given Tylenol for the pain, but I think Janet needed a shot of tequila more. On Thursday, Hailey was started on Sildenafil (a.k.a. Viagra…insert another little blue pill chuckle here). They’ve started her off at a relatively small dose of 1 mg per kg per dose, every 6 hours. After 2 days, they’ll start weaning her iNO. They’ll also closely watch her blood pressure. One of the side effects of Sildenafil is that it lowers the systemic (entire body) blood pressure. For Hailey that’s not necessarily a bad thing as her blood pressure has always been on the high side. |
July 6 - 12, 2009
|
No big changes this week.
She’s really starting to interact with us and her toys…and we discovered that she loves looking at herself in a small mirror that Janet put in her bassinet. After she’s been upset, we put the mirror in front of her – she seems to sooth herself like this. On Saturday, Hailey turned 2 months old. |
June 29 - July 5, 2009
|
A hearing test was done – all OK.
Other tests (metanephrines in her urine) were done to help determine if there is a reason for her higher than normal systemic blood pressures. OT also came by and showed Janet and her bedside nurse a Haberman bottle. It’s a bottle with a special nipple to make feeding with a cleft palate easier. Over the past week she’s had quite a bit of reflux (spitting up). To help, they are infusing her fed very slowly (over an hour) with a small pump. So far, so good – it’s helped. |
June 22 - 28, 2009
|
On the 23rd, we had a meeting with Dr. Pepelassis (Cardiology) and this week’s NICU Attending Neonatologist, Dr. Dakshimaurti.
When Hailey was originally admitted to NICU, she was diagnosed with having a patent foramen ovale (PFO) and a patent ductus arteriosus (PDA). A PFO is a defect in the septum (wall) between the two upper (atrial) chambers of the heart. Specifically, it’s a flap or a valve-like opening in the atrial septal wall. A PFO is present in everyone before birth, but seals shut shortly after birth. A PDA is a heart condition caused by the failure of the ductus arteriosus to close. The ductus arteriosus normally is a temporary blood vessel connecting the main vessel leading to the lungs (pulmonary artery) to the main vessel of the body (aorta). Normally, it begins to close immediately after birth. A significant portion of the general population has one of these defects (20% have a PFO and 10% have a PDA). Hailey was also diagnosed with having a bicuspid valve. It is a defect of one of the heart’s valves that results in the formation of two leaflets or cusps instead of the normal three. The heart’s valves ensure that the body’s blood only flows in one direction though the heart. A bicuspid valve, like Hailey’s, only happens in about 2% of the general population. Although any one of these heart defects can happen in a significant portion of the population, and any one of us can have one of these defects and not ever know about – our question Dr. Pepelassis was – and we were “stewing” over it for quite some time, but weren’t able to get an answer (until now) – what if someone, like Hailey for example, has all three of these. He told us that their latest cardiac echo showed that the PFO and PDA had almost totally closed. He then told us that he didn’t expect her bicuspid valve to be an issue until she was in her fourth or fifth decade – it took a few seconds for us to do the math and realize that that meant 40 to 50 years!! So in short – all three of her heart defects are a “non-issue” (at least for now). We also discussed performing a cardiac catheterization (“heart cath”). The heart cath would be used to help diagnose and determine the severity of her PPHN. While doing it, they would also try varying amounts of iNO and a drug called Sildenafil, more commonly called Viagra (insert chuckle here). Sildenafil helps dilate the pulmonary vessels in the lungs – similar to what the iNO does for Hailey. There are numerous risks to doing the heart cath (infection, blood clots that can trigger a stroke, damage to blood vessels, etc.). We also discussed not doing it until Hailey was 2.5 kg (she is currently 1.66 kg). Dr. Erikson (Nephrology) dropped by to examine her and look over her chart. Shortly after she was admitted, an exam showed that there were decreased flows through Hailey’s kidneys. Further tests and urine tests. Her urine samples looked good and her kidneys have grown. Another follow-up exam will be scheduled in a few months. Occupational Therapy (OT) and Physiotherapy (PT) also dropped by and showed Janet some stretches that we can do with Hailey. |
June 15 - 21, 2009
|
Hailey was having pretty consistent “water loss” in her stools (i.e., diarrhea), so on the 16th her milk additive was changed to “Progestimil”.
On the 17th, Janet turn 29... at least that's the age she told everyone. On the 19th, another cardiac echo was done. It showed increased pressures in the heart and an enlarged right side. Her PPHN remains her main fight for now. Her iNO was increased to 10 ppm. |
June 8 - 14, 2009
|
Through the week, she had increasingly large amounts on “gunk” around her eyes, so they started her on eye drops to help clear it. It worked – within a couple of days we could see her beautiful eyes again.
They “lost” her IV on the 8th. Instead of starting another IV, they orally gave her Amoxicillin. The lab results came back on the 9th and didn’t show anything, so her antibiotics were discontinued. During the many prenatal ultrasounds, it was suspected that Hailey had Russell-Silver Syndrome (RSS). Shortly after she was born, Dr. Chodirker examined her - this further reinforced his suspicions. He sent away blood samples from Hailey, Janet and Colin. At that time, he said that we might get the results back between 2 weeks and 6 months…well we got them back this week. Yes she does have RSS – to be precise, she has H19 Hypomethylation (also known as 11p15). Read more about it here. Of course this isn’t fantastic news, but at least we know for sure what has caused and is continuing to cause her growth retardation. On Thursday, Hailey turned 1 month old, and her Gigi turned 79 years young! |
June 1 - 7, 2009
|
Her iNO was weaned down to 2 ppm by the 5th. Then to 1 ppm by the 7th.
On the 4th, “beneprotien” was added to her milk to help increase her caloric intake. She was suspected of having another infection on the 6th, so another IV with antibiotics was started. This time, she was able to stay in her bassinet. |
May 25 - 31, 2009
|
On CPAP until the 27th, then on nasal prongs (NP). Also on the 27th…all clear – the results came back from the lab; no infection. So the IV was stopped and she was also moved back into her plastic tub…urr…bassinet.
On the 28th, the results of a cardiac echo (an ultrasound of her heart) came in; she was diagnosed with Persistent Pulmonary Hypertension of the Newborn (PPHN). This is a condition where blood moving from the heart can’t move through the lungs properly. This can cause her heart to over work and become enlarged. On the 29th, they started her breathing a gas (along with regular room air) called Nitric Oxide (iNO). She was started off at a moderately low rate of 10 parts per million (ppm). The iNO is breathed into the lungs and helps open the small pulmonary vessels to allow the blood to move more freely through the lungs. |
May 18 - 24, 2009
|
On the 20th, Janet got to hold Hailey “kangaroo cuddle” for the first time – Hailey lying on Janet’s chest (skin to skin).
The heat part of Hailey’s isolette was turned off on the 22nd – she was producing enough of her own heat that she was getting too hot in the isolette. She was on CPAP until the 23rd, then on nasal prongs with room air (i.e., no additional oxygen). Also on the 23rd, she was moved from her isolette to a bassinet (i.e., a plastic tub). Then a bit of a step backwards…on the 24th, they suspected that she had an infection. So they started an IV in her arm so that they could administer antibiotics. The IV was almost as big as her!! Also because of this, she couldn’t be dressed the same – so she was put into a “radiant warmer” isolette. Then to top it off…back on CPAP. During Hailey’s initial intubation, they noticed that she has a posterior cleft palate. It’s definitely into the soft palate, but it’s very difficult to tell how far, if at all, her hard palate is affected. It doesn’t go though her jaw or into her lip. A nurse from the cleft palate team dropped by to talk to us. Once Hailey is more stable, they’ll take a closer look at her, but it sounds like they won’t do anything for several months. An upside is that her dental will be covered by Manitoba Health for the rest of her life. |
May 17, 2009 (Sunday)
|
Hailey had her first real bath!! Nurse “Auntie” Cathy turned it into a day at the spa by making her a “spa turban” from a wash cloth and took pictures (we’re sure they’ll resurface a little later in her life…)
Later that evening, we had a bit of a scare as she “desatted” (her blood oxygen levels dropped) pretty badly twice, resulting in…back on CPAP later that night. |
May 16, 2009 (Saturday)
|
Off CPAP…
Hailey also had her umbilical arterial and venous catheters (central lines through belly-button) removed. There is a fear that leaving them in too long can lead to a nasty infection as they almost go into the heart. A skin temperature probe was also removed as it wasn’t working all that great anyway. |
May 15, 2009 (Friday)
Back on CPAP…
May 14, 2009 (Thursday)
|
Hailey was taken off CPAP – as we would shortly learn, this would be the first of many “trials”.
Hailey started feeding Janet’s breast milk today. At least for now she’ll be fed through a small tube that is inserted through her mouth and down her throat – called an oral gastric tube or OG (the same tube is called a nasogastric tube or NG when it runs through the nose). Her milk is “infused” very slowly with a syringe. In the beginning, she’ll be fed smaller amounts and supplemented with sugars (etc.) through her IV. With a couple of days, she’ll be on “full feeds”. Today was a crazy busy day – Janet was “released” from the hospital. On the way home, we needed to go shopping for some “supplies” for Janet and Hailey… and, due to some extremely bad timing, our fence posts were installed. |
May 13, 2009 (Wednesday)
|
First thing in the morning, Colin went over to check in on Hailey. Through the night, they decided that she needed to be put on CPAP (meaning Continuous Positive Air Pressure) – it’s similar to a sleep apnea machine, and keeps positive air pressure in the lungs to help her breathe.
Colin was pleasantly surprised to be “offered” to hold Hailey for the first time – even though he knew that this would make Janet extremely jealous, he jumped at the chance. A little later, Janet and our friend, “Auntie” Chantel, came to NICU and Janet got to hold Hailey for her first time – and Chantel took our first family portrait. |
May 12, 2009 (Tuesday)
|
Somewhat refreshed, and ready to tackle our reality of being new parents of a baby in NICU, Colin made his way over to Women’s Hospital to meet Janet, then the two of us made our way over to NICU.
There we were pleasantly surprised to see that Hailey was off the ventilator and was breathing “room air”. We were able to see our baby girls face “unobstructed” for the first time…we have the cutest kid!! During her lunch break, Auntie Cathy came to meet Hailey. Then, during the evening, Auntie Lynne, Uncle Paul and cousin Evan came to visit. |
May 11, 2009
|
WOW!!! Today’s the “big day”!!! Still kinda weird knowing (nearly) the exact time and day that our baby will be born.
The day started at 6:00ish with a little less than 4 hours of sleep. We needed to be at the Woman’s Hospital admission desk for 8:00…unusual for us, but we made it on time. After being admitted, we were sent up to Prenatal Triage in the High Risk Delivery area. There, just another example how small Winnipeg can be, the nurse looking after us is our neighbour’s mother – she recognized our address. Janet got changed and they did the usual pre-op. work-up (blood pressure, etc.). Marie (from Fetal Assessment) came by to do one last ultrasound - just to confirm that the baby hadn’t turned to a head-down position – it didn’t. Then we waited…aarrrggg…it seemed to take forever for 10:00 to roll around…that’s when time started to fly! Janet was whisked off to the Operating Room and Colin was given a chair in the hallway while they got Janet setup and ready to go. It seemed to take forever…he was beginning to wonder if they forgot about him!! Not quite, Dr. Logan hadn’t arrived. As Dr. Logan was washing to go into the OR, she asked Colin “So? Do we have a name for this little girl yet?” Colin replied, “Oh? Is that what we’re having?” Dr. Logan soon realized that she let it slip and tried to backtrack, but it didn’t work. Now Colin had to bite his tongue for the next little while until Janet could see the surprise for herself. Once Colin was escorted into the OR, Janet was already prepped and ready to go. Colin was given a stool near Janet’s head (both of us – Janet’s head at least – were behind a curtain). We were able to watch the whole thing in a mirror above the table. Janet said that it felt like an out of body experience or that it was on TV, because she couldn’t feel anything except for the occasional tug or pull. It took just a minute or so before they were pulling our little baby girl out into the world. Except, she didn’t want to come…her head didn’t want to come out…a quick little extra snip, and out she came. She was quickly whisked across the hall to a Resuscitation Room where a team of doctors and nurses were waiting for her. Because of the unknowns of what was going on with her, they wanted to be prepared. In the Resus Room, they weighed her (1 338 grams or 2lbs, 15.2oz. including her endotracheal tube and umbilical arterial and venous catheters!!) and began assessing her. She needed a little help with her breathing, so she was intubated and put her on a ventilator. Later we would be told that the ventilator was set at its lowest setting and that she only occasionally needed its help. As Janet was being “sewn” back up, Marie (from FA) took Colin across the hall to meet the baby and take her first pictures. Soon after that, Colin was taken to Janet’s recovery room and Janet soon joined him (wheeled in of course). Between many, many tears of joy, happiness and uncertainty, we picked her name, Hailey Marie Paterson (see below). Shortly after that, Auntie Lynne joined us in the recovery room…then we waited and waited and waited. It seemed to take forever!! It almost did…a very long 2 hours and 40 minutes. Then, Baba (Janet’s mom) and Auntie Debbie showed up in the recovery room…just mere seconds before Hailey was wheeled in. Janet finally got to meet and touch Hailey for the first time. It was brief, but she was able to touch her through the port of “the cart”. Before Hailey was born, there was some doubt where Hailey would go. If everything was good, she would join Janet on the ward in Women’s Hospital. If she needed help breathing, she would be transported to the NICU in Children’s Hospital. If she just needed minor support and monitoring, she would be moved to the T1 (Intermediate) Nursery. Because she was on a ventilator, she needed the NICU. “The cart” is a little self-contained intensive care unit on wheels and was how Hailey was transported from the second floor of Woman’s Hospital, through the subterranean tunnels of HSC to the NICU on the fourth floor of Children’s Hospital. “The cart” had everything Hailey needed for her first road trip – a ventilator, IV pumps, monitors and heat for the isolette (incubator). In all it took about 12 minutes to make the trip with Hailey in “the cart”, her team of Doctors and nurses…and dad in tow. Once there, Colin was given a seat in the “Parent Lounge” while Hailey got settled into her new “home away from home”. A window seat…bed number 3 in Module A. Once Hailey was settled, Dr. Chiu (an NICU neonatologist) and her first (admitting) nurse, Dave, gave Colin an update and helped get rid of that “freaked out dad look” as they tried to reassure him that she was good and was in good hands. After some more “finger cuddles” with Hailey and more pictures, Colin left to navigate his way back to Women’s Hospital and try to find Janet. Meanwhile, after Janet got most of the feeling back in the lower half of her body, she was wheeled over to the third floor of Women’s Hospital and lucky for us, into a “private” room. She was joined by Baba and Gigi (Janet’s mom and dad), Auntie Lynne and Auntie Debbie. Colin was able to find them, and gave his “report” to the “new mommy” and the rest of the family…and of course showed all of the pictures taken thus far (the first of many, many, many more to come). After dinner, Gramma and Papa (Colin’s parents) came for a visit, and the proud daddy took them over to NICU to meet their newest granddaughter. When they got back to Janet’s room, Uncle Darrell and Auntie Debbie were there for a visit. Janet was feeling good, so the four of us made our way over to NICU. By this time Colin’s shoes were wearing out from all of the miles back and forth through the tunnels. But of course it was all worth it!! By this time, Janet and Colin were beyond exhausted!! Janet settled in for the night and Colin went home to “relieve” the dog (and cat). Before bed, Colin sent out the “press release” – as mass email to over 160 of our closest family, friends and colleagues. About "Hailey Marie" Once Janet was in the recovery room, between tears, we were finalizing names. We were pretty set on Hailey (obviously if “Bubba” turned out to be a girl). But we were still somewhat undecided on her middle name. About a week before the “birth date”, Colin threw out “Marie” for a middle name. Marie was the nurse that did most (all but one) of our ultrasounds in Fetal Assessment. Even though we got unbelievable support and encouragement from our families and friends, we cannot even begin to imagine how much more difficult this “adventure” would have been without the support and advice that we received from Marie. She went “above and beyond” our expectations. At every twist and turn..yes, she was honest and told us what she was seeing that was “abnormal”, but she also took exceptional time to show us “the good” that she was seeing and why that was so important. She also took us on tours of the T1 (Intermediate) Nursery, High Risk Labour, OR and recovery rooms. Then to top it off, she sat with us (more like held our hands) during the entire delivery. Then while Hailey was in the resuscitation room, she kept us updated with what was going on and her progress. So it was set…from now on, our new little baby girl would be known as Hailey Marie Paterson. |
May 10, 2009
|
WOW!!! Tomorrow’s the “big day”!!! Although we didn’t expect our baby to come home with us, we still spent the day getting final touches done on the baby’s room…getting furniture assembled and in place. Then Colin got into preparing the web site and email for the coming big announcement…our “press release” as it became known as. Between family, friends and colleagues, the initial email was to be sent to over 160 people…even that was trimmed down. Needless to say, it took a bit of effort to assemble an email for that many people. For whatever reason…call it nerves, make-work projects or disorganization, we didn’t get to bed until 1:00 in the morning. Even at that, it was well after 2:00 before we turned the lights off...
|
Background
|
Of course we were very excited to learn that we…urrr, Janet was pregnant. But there was soon to be some trepidation after Janet’s Ob/Gyn (Dr. Logan) sent her for some very early ultrasounds after a routine blood test showed some concerns. At that point everything looked normal as any “grain of rice” might look via ultrasound.
Then came the “triple scan” (a blood test for Downs Syndrome, Trisomy 18 and Smith-Lemli-Opitz Syndrome). We debated the pros and cons of having the triple scan done. A couple of friends warned of the frequency and overwhelming stress that can come from a false positive result. With consultation from Dr. Logan, we decided to go ahead with it. Her advice was that it might be better to know and be given the opportunity to plan for something opposed to it being a complete surprise on the day that the baby is born. A couple of weeks after the test (sometime in early December), after almost forgetting that we did it, we got an urgent call from Dr. Logan saying that there were significant concerns with the results and asked that we go to Fetal Assessment at HSC the following afternoon. At Fetal Assessment, we first met with a genetics doctor (Dr. Chodirker) who asked us for our family histories and asked questions like “Are you cousins?”. He then got into the results of the triple scan. The scan results don’t give yes and no answers, but odds. For Downs it was something like 1 in 250, not terribly far off of the odds for Janet’s age (the average for a 35…ur…29 year-old woman is in the order of 1 in 300). As for Trisomy 18 and Smith-Lemli-Opitz Syndrome, our results were 1 in 7 and 1 in 6. Needless to say that at this point in the conversation, we were pretty distraught, upset, worried, etc., etc. We then moved to an examination room to complete an ultrasound with Marie Hadfield, R.N. and Dr. Reid. After several very anxious minutes, measurements and “hmms” and “ahhhs”, they told us that something was wrong with the baby, but that they couldn’t tell us what it was or the severity. Based on the measurements, the baby’s head size was near normal, but the body and limbs were several weeks behind. They proposed that they do an amniocentesis to help determine a diagnosis (or rule out some possibilities). After briefly contemplating the risks, we decided to go ahead with it…but we wouldn’t hear about the results until right before Christmas. It would either make it a really good Christmas or a really sucky one. So after several anxious, sleepless weeks, on Christmas Eve day, we received a telephone call from Dr. Chodirker with results. All was good…except (sounds of flipping through papers)…one result was missing…the one for Smith-Lemli-Opitz Syndrome. Arrrggg…we wouldn’t hear about it until after Christmas. The week between Christmas and New Year’s, we were scheduled for another ultrasound. The results for the Smith-Lemli-Opitz Syndrome test were waiting for us, and was OK. The ultrasound showed that the baby was doing good, but there was still a discrepancy between the head and body size. The baby’s posture and movements were all normal. They still didn’t know what, if anything, was wrong. During a February ultrasound, Dr Reid spent an awfully long time looking at the baby’s heart. We each had a feeling that something must be wrong. It seemed like hours…we kept squeezing each other’s hand and sharing anxious looks. After the ultrasound examination, he asked that we meet with him in a consultation room. There, he told us that the baby has a hole between the left and right atriums. He reassured us that it was not a major hole, and that a significant segment of the population has this condition and may not even know it. However and obviously, we still were concerned. At one of the appointments (at the beginning of March), Dr. Chodirker (genetics) met with us again. Apparently he recently returned from a conference where someone made a presentation on Russell-Silver Syndrome, and he thought that our baby might have this. We were quite sceptical. Had someone presented another syndrome, might our baby have that?... He reassured us that based on the symptoms and normalities that they were seeing, Russell-Silver fit the picture. He explained and showed us some literature of what Russell-Silver is and what the prognosis might be. As with any syndrome, the prognosis and severity varies from individual to individual. He also explained that we wouldn’t not know for sure if the baby has Russell-Silver until after the baby was born and further tests could be done, or, the possibility, that we may never know what was wrong. At this point we felt quite relieved. For one, at least we had an idea of what might be wrong. There was always some doubt because it could still be something else. But at least we had a direction to go towards. After some more research and based on what Dr. Chodirker told us, we decided that if our baby had to have a genetic disorder or physical disability, Russell-Silver might be the one to have. With the exception of being physically smaller, most people with Russell-Silver can lead pretty normal lives. Yes, there would be some difficulties and challenges, but something that we can all cope with. In all, we had about 8 ultrasounds at Fetal Assessment, each showing the same thing – normal sized head and small body and limbs. Getting towards the due date (May 16th), the ultrasounds showed another concern…the baby hadn’t turned to a head down position. Due to the size discrepancy between the head and body, they had concerns about delivering the baby breach. They also didn’t want Janet going into Labour and putting the baby under stress...so, they wanted to schedule Janet for an “elective” Caesarian Section one week before the due date. Janet called Dr. Logan’s office to make the appointment. They tried for several days before and after the target date (May 9th), but nothing was available. The best date was May 14th, just 2 days before the due date. Then a few days later, we got a call from Dr. Logan’s office…they rescheduled us for May 11th at 10:00 am…kinda weird knowing the exact date and time that your child will be born. |